From the Open-Publishing Calendar
From the Open-Publishing Newswire
Indybay Feature
2016 San Francisco Workers Memorial Day

Date:
Thursday, April 28, 2016
Time:
7:00 PM
-
9:00 PM
Event Type:
Panel Discussion
Organizer/Author:
Injured Workers National Network
Location Details:
ILWU Local 34 (next to AT&T Ballpark
801 2nd St. San Francisco, California
801 2nd St. San Francisco, California
2016 San Francisco Workers Memorial Day
Remember The Dead And Fight For The Living
Defend Our Health & Safety Rights And Our Lives And Families
Thursday April 28, 2016 7:00PM
ILWU Local 34 (next to AT&T Ballpark
801 2nd St. San Francisco, California
April 28 is Workers Memorial Day and is commemorated throughout the world for workers who have died or been injured on the job and to fight for health and safety on the job for workers and the public.
In California workers die nearly every day because of the lack of health and safety protection and many are sickened by toxins and workplace bullying on the job which is reaching epidemic rates.
There also have been incidents of =93hanging nooses=94 put up on worksites at SF Recology and the Bay Bridge to terrorize and intimidate African American and other workers.
At the same time there are only 200 Cal OSHA health and safety
inspectors for 18.5 million workers in the State and only 2,000 for the federal government. We need to demand that there be proper enforcement for health and safety violations including jail for deaths caused by violating health and safety laws.
Additionally as a result of deregulation of workers compensation in California under SB 899 and SB 863 seriously injured workers have to go through hoops and a system called independent medical review to get medical treatment and the insurance controlled Workers Comp system stalls treatment and instead doctors in many cases are forced to
prescribe opiate drugs that end up addicting injured workers and
destroying their lives.
Under Federal and California law, workers union and unorganized are supposed to be protected when they complain to OSHA about health and safety violations. The reality is that companies and bosses regularly
bully, harass and fire workers who fight for their health and safety for themselves and the public.
Federal OSHA lawyer Darrell Whitman who was investigating retaliation complaints at PG&E, Fed Ex, Test America, Lockheed Martin and other companies found that there was illegal retaliation and then OSHA management with the backing of DOL Secretary Of Labor Tom Perez. OSHA managers bullied and harassed AFGE investigators and lawyers in the Whistleblower Protection Program and illegally fired Whitman for trying to defend OSHA whistleblowers. We will discuss what workers can do to protect their rights and get justice and accountability.
It is time to remember the dead and fight for the living. We have a
right to work in a healthy and safe workplace for ourselves and our
families.
Initial Speakers:
Brenda Barros, SEIU 1021 SF General Hospital Chapter Chair
Dr. Larry Rose, Past Medical Director of Cal-OSHA
Daryle Washington, IBT 350 Worker At SF Recology
Daniel Berman, Health and Safety Advocate and author of =93Death on the Job
Dorian Maxwell, Fired MTA TWU 250A bus driver and OSHA whistleblower
Roland Sheppard, Retired Painters Local 4 BA
For more information Injured Workers National Network
http://www.iwnn.org
Endorsed by
SMART UTU 1741, IWNN, UPWA
https://www.facebook.com/Injured-Workers-National-Network-=85/
(415)282-1908
info [at] iwnn.org
Billion Dollar Scam In California Workers Comp System Destroys Workers And Bilks The Public
https://www.revealnews.org/episodes/billion-dollar-scam/
Apr 2, 2016 SHARE
California’s workers’ compensation program covers 15 million workers across the state. If you get hurt on the job – fall off a ladder, for instance – it’s the system you turn to. Most employers are required to carry workers’ comp insurance, which helps cover medical bills and lost wages for injured employees.
But Reveal reporter Christina Jewett has discovered serious fraud in the system after reviewing thousands of documents. They show that in the last decade, more than 80 people have been accused of cheating California’s workers’ comp medical system out of $1 billion.
Jewett and producer Delaney Hall tell the story using an undercover law enforcement wiretap and the accounts of a worker, employer and investigator.
Host Al Letson then sits down with Jewett to really dig into what it is that makes workers’ comp such an easy target for people who want to take advantage of it.
And finally, we revisit a story about the bogus screws that ended up in spines of surgery patients. You can consider it the prequel to the main investigation …
Profiteering masquerades as medical care for injured California workers
https://www.revealnews.org/…/profiteering-masquerades-as-m…/
By Christina Jewett / March 31, 2016
Priscilla Lujan was awake soothing her infant son at 10 p.m. and again in the middle of the night. She let him gum one of the salty pistachios she was eating. She mixed a bottle of formula at the side of their shared bed.
It was the fitful kind of night that’s easily forgotten after a strong cup of coffee and a shy smile from a sleep-refreshed baby.
But that’s not what happened the next morning. When Lujan woke up, her son – not yet 6 months old on Feb. 3, 2012 – was cold. His lips, blue. His eyes, half open. She screamed to her mother to call 911.
At the hospital, Lujan stood in a room rocking her baby from side to side, sobbing. By then, Andrew Gallegos already was dead.
Police showed up at Lujan’s East Los Angeles home about a week later – more than a dozen of them. They seized her medications. They handcuffed her and drove her to the police station, where a detective demanded answers: Why did her baby have toxic levels of pain medicine in his bloodstream?
During the interview, it dawned on Lujan: The pain cream she had slathered on her knee had gotten into her son’s mouth, through the pistachio and bottle of formula.
Photos of tubes of pain cream seized from Priscilla Lujan’s home were presented to an Orange County grand jury. Prosecutors alleged that businessman Kareem Ahmed helped formulate the toxic cream and was culpable in the death of Lujan’s infant son.
Credit: Orange County Superior Court
“Oh my God, I killed my baby,” she told the detective.
Soon after, the focus of the case shifted. The new target was Kareem Ahmed, a millionaire businessman who made his fortune selling medicated creams for patients like Lujan, who struggled with pain after an injury on the job.
Ahmed eventually would be indicted for involuntary manslaughter in Andrew’s death and accused of a far more sweeping crime: paying more than $25 million in bribes to doctors, including Lujan’s, who prescribed the pain-relief creams.
To the people who combat fraud in California’s $24 billion workers’ compensation system, the case exemplifies unchecked profiteering that jeopardizes injured workers’ health and lives.
It is one of more than a dozen cases that, taken together, outline a medical landscape in which corruption masquerades as medical care for some of California’s injured workers.
A review of thousands of criminal court records by Reveal from The Center for Investigative Reporting shows a system in which pay-to-play schemes trump patient care, particularly in unregulated treatments rejected by insurers and disputed in obscure courts throughout the state.
Prosecutors are beginning to turn the tide, pursuing charges against more than 80 medical professionals who’ve handled more than 100,000 injured-worker cases, most of them originating in Southern California.
Defendants include a physician assistant accused of “aggravated mayhem” after he operated on dozens of injured workers’ knees and shoulders, despite lacking surgical training. The outcomes often were disastrous.
“It still hurts today,” one worker testified in 2015, describing his unsuccessful 2010 shoulder surgery through an interpreter. “I can’t, you know, bend my arm, really.”
Along with the court records, Reveal analyzed data from more than a million workers’ compensation court cases, which show that over the last decade, workers have been swept into medical billing mills, prescribed unregulated medications and advised to undergo sometimes unneeded or high-risk surgery by doctors who were raking in bribes.
RATHER LISTEN TO THE STORY?
Subscribe to the Reveal podcast to get this and other stories.
Prosecutors estimate that the accused have burdened the system with more than $1 billion in demands for money intended to help injured workers get back on the job.
The cases are being fought vigorously at every turn. Ahmed’s attorney secured an early victory, getting all but one count in his indictment thrown out; the prosecutor says she will refile the charges. Other attorneys defending the accused say the barrage of cases is a witch hunt that scares medical providers away from the system, limiting workers’ access to care.
Taken together, the alleged schemes inject cynicism into a system in which workers already are at odds with insurers, which can save money when they deny care. They heap costs in the form of higher premiums on employers, who in turn raise prices for goods or services or stem hiring as they pay the highest workers’ compensation rates in the nation.
Workers such as Tammy Martinez, though, pay the greatest price. The 56-year-old truck driver hurt her back pushing a 1-ton cart.
The workers’ compensation attorney whom she relied on to help her navigate the system pleaded guilty in 2014 to being part of a criminal club: people taking bribes from hospital executive Michael Drobot.
Drobot had pleaded guilty in early 2014 to paying at least $20 million in kickbacks to dozens of marketers, doctors and others who helped him fill the surgery suites at the now-defunct Pacific Hospital of Long Beach. Federal prosecutors linked the bribes to more than 4,400 risky spinal operations at the hospital.
Martinez’s lawyer, Sean O’Keefe, recommended that she see a surgeon, who, she later would learn, also was accused of taking bribes from Drobot. O’Keefe’s guilty plea singles out Martinez’s case as one spurred by illegal bribes and a conspiracy compelling her surgeon to perform a particularly complex – and expensive – operation.
Michael Drobot, executive of the now-defunct Pacific Hospital of Long Beach, pleaded guilty in 2014 to paying at least $20 million in bribes to bring spinal surgeries to his hospital.
Credit: Pacific Hospital of Long Beach website via Archive.org
When it came time for Martinez’s spinal surgery in October 2011, all did not go well. Doctors noted that after the procedure, her left foot grew pale and pulseless. Within weeks, her leg had to be amputated above the knee.
Since then, she said, it’s been a difficult journey to learn to stand again and to discover that her young grandson was not, in fact, afraid of her.
“I lost myself,” Martinez said. “I struggle every day to get the person I used to be back.”
Across Southern California, Reveal found, companies employ intensive marketing to tap into a particularly vulnerable segment of the workforce. They blanket Spanish-language media with ads and target Latinos with calls to their homes. They suggest that filing a case could lead to a windfall.
“Receive up to $4,000 per month,” proclaim Spanish-language signs, business cards and fliers posted across Southern California. One workers’ compensation attorney troubled by the ads called the number out of curiosity. After that, messages from a buzzing call center lit up his phone five times a day – for months.
Callers wanted to know “if I knew anyone who had been injured,” San Diego attorney John A. Don said, “if I could refer anyone to them.”
Christine Baker, director of the state Department of Industrial Relations, which administers workers’ compensation, initially responded to questions with a statement noting that other state authorities oversee medical providers and health fraud. But two weeks ago, she said her department had taken a closer look at unregulated medical care, and “we know there’s a problem.”
“We want workers to get appropriate care,” she said. “We don’t want overcare or undercare; either way is wrong. Delivery of care needs to be evidence-based, appropriate and quickly delivered.”
Baker said medical abuse is a symptom of a “deeper problem,” particularly in Southern California.
There, workers’ comp stands out as an easy target for scammers. While health care programs such as Medicare have developed an arsenal of weapons to ward off fraud, California state regulators have few tools at their disposal. For one thing, the state shares oversight with hundreds of insurers and self-insured employers, leaving no one clearly in charge.
Prosecutors filing a growing parade of cases are exposing this leadership vacuum and how it allows operatives to bypass the most competent medical providers for the highest bidder. Workers who’ve been hurt on the job often are the last to find out that they have been exploited – if they find out at all.
“We’re talking about a patient that has become a commodity,” said Don Marshall, chairman of the state’s Fraud Assessment Commission, which distributes funds to prosecutors who fight workers’ compensation fraud. “It’s become something to trade and sell on the open market for no other reason than to generate income.”
‘Nobody cares’ about workers’ comp
As investigators began to puzzle over the 2012 death of Andrew Gallegos, it did not take them long to realize they already had a window into the world of the man who ultimately would be charged in the case.
Businessman Kareem Ahmed has been accused of paying more than $25 million in kickbacks to doctors in a workers’ compensation fraud scheme.
Credit: Paul A. Hebert/Invision/AP file
Kareem Ahmed was the owner of Landmark Medical Management. He is not a pharmacist. But prosecutors, in the continuing legal case against him related to Andrew’s death, would point out that he still delved into the science of mixing medications to formulate pain creams.
Ahmed’s goal, they allege, was not to make the most effective salve, but the most profitable one. Experts would testify that, if ingested, the opioid-infused cream was a “loaded gun” that could kill an adult. His firms billed insurers $400 to $1,700 per tube for creams sent to Priscilla Lujan, totaling $59,000, court records show.
An undercover recording made nearly four years before Ahmed’s indictment gives a wider view of the world of workers’ compensation medical executives. In that recording, Ahmed makes it clear that many of them are up to no good – and no one is stopping them.
Businessman Cyrus Sorat secretly recorded the conversation. Also in the pain cream business, Sorat was working for federal prosecutors as part of an agreement to seek leniency in a separate workers’ compensation fraud case.
As the two men shared a leisurely lunch at an upscale restaurant in Ontario, California, Ahmed marveled over the scale of the exploits of others who, like him, made their millions off health care for injured workers.
One stood out, he said, for paying doctors up to $50,000 a month to perform invasive and risky back surgeries: Drobot, the Long Beach hospital executive who eventually would plead guilty to bribing the surgeons.
“How come nobody does anything to him, man?” Ahmed implores in the recording, pounding the table.
When it comes to workers’ comp, nobody cares.”
— Kareem Ahmed
owner of Landmark Medical Management, in a secretly recorded conversation with businessman Cyrus Sorat
Sorat lowers his voice. “Let me tell you something. If you do Medicare – the feds hang you,” he says.
“Oh, I know, that’s why I never touch Medicare,” Ahmed says.
“But when it comes to workers’ comp, …” Sorat continues.
“Nobody gives a fuck,” Ahmed finishes the sentence.
“Nobody cares,” Sorat agrees. Ahmed laughs.
The men go on to discuss other workers’ compensation moguls. They cluck about a former chiropractor who they say had gotten a multimillion-dollar settlement from a large insurer. Sorat calls him “a criminal.”
SIGN UP FOR OUR NEWSLETTER
Stay up to date with the latest investigations and episodes from Reveal delivered to your inbox.
“Yeah, and then he gets money. He’s wanted in six different states,” Ahmed said. “But nobody did anything. … Nobody does shit.”
They also talk about David Wayne Fish, a businessman who pleaded no contest in 2010 to taking money for patient referrals. He was accused of organizing dozens of lawyers and doctors to steer more than 4,000 cases to preferred medical providers and run up high bills.
Fish’s sentence: probation, fines and an order to stop demanding the $60 million he was seeking from insurers.
“He’s … walking! What happened to him? Nothing,” Ahmed said. “Six fucking years of (investigation), thousands of hours, and he’s walking? … He’ll … make a $100 million in one year again.”
“When it comes to workers’ comp, …” Sorat said.
Ahmed finished his sentence once again: “Yeah, nobody cares.”
Abuse abounds in specialized courts
On a sunny Monday in November, the workers’ compensation court in Marina del Rey is swarming with activity. Lawyers weave down the halls from small courtroom to courtroom and gather in clusters. Others fervently broker deals on their cellphones.
There are 24 courts like this up and down the state. But the activity is particularly frenetic in Southern California, where the paperwork that fuels the court’s pace comes in by the virtual truckload.
Christine Baker, director of the California Department of Industrial Relations, says her department has taken a closer look at unregulated medical care, and “we know there’s a problem.”
Credit: California Department of Industrial Relations
These courts spend the bulk of their time settling liens – claims for payments that medical and other service providers file against insurers or self-insured employers.
The lien system was created to protect the injured worker. It guarantees that even if insurers deny medical care, workers will have a medical professional to whom they can turn.
But the system also throws its doors open to providers excluded from insurers’ networks of preferred professionals. It allows thousands of unregulated entities to bill for any treatment, whiz-bang device, pain cream or DNA test. The only limit is the providers’ willingness to roll the dice on how much money they’ll rake in at workers’ comp courts.
The lien system thrives in California – more than in any other state. One national insurance executive estimated in 2010 that his company does one-fifth of its business in California – but deals with more than four-fifths of its liens there.
That volume creates “a very thick forest for thieves and scoundrels to hide out in,” said Lachlan Taylor, a former special counsel to the Department of Industrial Relations who analyzed the lien system in 2010.
His work informed a 2012 law that cut down on liens with a new $150 fee required to demand payment in workers’ compensation courts. It also gave insurers new powers to deny money to providers that aren’t approved to treat injured workers.
Yet claims for unapproved care still are cropping up, said Baker, the Department of Industrial Relations’ chief. And the number of liens filed last year is even higher than it was when Taylor initially concluded that the system “rewards bad behavior.”
Baker said her department has begun reviewing the medical providers who currently file the largest number of liens. The result: “We do note that many are (criminally) indicted.”
The shifting array of schemes is difficult for government authorities to track, much less for workers such as Denise Rivera. Her medical care providers amassed bills – or liens – amounting to $95,000. Yet the knee she sought help with continues to ache, swell and give out.
She injured it while working at a center for severely disabled children, a nursing assistant job she loved. She worked the night shift, feeding children, turning them when they slept and getting them ready for the next day.
“When you came in, (the kids) had a smile for you,” said Rivera, who lives in Riverside County.
Two days after Thanksgiving in 2011, she slipped and fell while giving a child a shower. Rivera said she immediately felt paralyzed by leg and back pain. Her company’s doctor said she needed knee surgery, but her employer’s insurance company denied the request.
Rivera saw a commercial on TV for legal help with a work-injury case, called the number and got connected to California Injury Lawyer Inc. The Corona-based company sent people to her house to take her information and referred her to a Riverside clinic, she said.
They’re intrusive. I have people tell me that they’ll call every single day.”
— Teena Barton
ICW Group Insurance Cos. special investigator, on marketers and advertisers
Teena Barton is familiar with this kind of advertising through her work as a special investigator in San Diego for the ICW Group Insurance Cos., a workers’ compensation insurance firm.
Barton said marketers and advertisers are invasive, often pressuring workers to refer friends and co-workers, who get cold calls at home. She said workers often are pressured into filing work injury claims and put on a lengthy course of medical treatment.
“The problem is once you’re on that wave, that wave’s going to take you,” Barton said. “That’s what the system is. ”
Multiple medical procedures
The people who asked Denise Rivera, 54, to sign papers advised her to report to a Riverside clinic, she said.
The clinic packed her schedule with appointments. Clinic staff gave her what looked like a school lunch menu, with the names of doctors and companies she was expected to see three times per week.
Rivera cobbled together the gas money or borrowed family members’ cars to make her appointments. She sat in the clinic’s jammed waiting room for hours at a time and watched medical staff wheel in suitcases full of devices to treat workers.
Denise Rivera said she didn’t work for four years while waiting for her workers’ compensation case to be resolved. She ultimately got a settlement for $32,500 – about a year’s pay.
Credit: John M. Blodgett for Reveal
She said she received MRIs, acupuncture, shockwave therapy and treatments with a device that seemed like a jackhammer thumping her knee. At one point, clinic staff sent her home with an electrical pain treatment device, but they forgot to include the electrode pads needed to make it work.
Pain creams that “seemed like Bengay,” according to Rivera, arrived in the mail. For those creams alone, records show that Kareem Ahmed’s company billed $17,102. Ahmed is the pain-cream executive who was charged in baby Andrew Gallegos’ death. The pharmacist who made 145,000 tubes of cream for his company got $35 to $72 per tube, public records say.
Records in Rivera’s case show the total bill sent by providers to the insurer for her care: $95,257. She had never seen that total, and it shocked her.
“No way,” she said, then added: “None of the treatments they’ve given me has helped.”
Rivera said she did not work for four years while waiting for her workers’ compensation case to be resolved. Penniless, she set up her bedroom in her mother’s garage.
She ultimately got a settlement in the case to compensate her for a permanent disability. The amount was $32,500 – about what she would have made in one year at work.
Going after ‘The Godfather’
Riverside County prosecutors now allege that Rivera walked into a clinic, with eight affiliate sites, that ran a $122 million scam.
They filed charges in July 2014 against attorney Cary Abramowitz and chiropractor Peyman Heidary. Prosecutors say in court records that Heidary is nicknamed “The Godfather” for masterminding the profit-centered medical network that Rivera encountered.
Heidary is accused of controlling medical treatment at the clinics, even though he’s not a doctor, which is a crime in California. Prosecutors say he also illegally owned and controlled law offices, even though he’s not a lawyer.
Prosecutors claim that workers came into the network via “cappers” – people paid to recruit patients – who got referrals from English- and Spanish-language 800 numbers. At Heidary’s direction, clerical staff allegedly padded the cases with additional supposedly injured body parts, according to court records.
Of the $122 million Heidary’s group sought, one document from prosecutors indicates that it had collected $18 million from insurers as of April 2015.
Rivera said the allegations were bad news for her, given that she trusted the legal and medical professionals to fight for her best interests.
“It makes me angry,” she said. “I kind of want to cry.”
Basically, I got screwed.”
— Denise Rivera
former nursing assistant
Heidary has pleaded not guilty. His attorney, Michael Khouri, said the case lacks legal and factual merit and has ruined Heidary’s reputation. All the care, he said, was medically necessary.
When told about Rivera’s plight, Khouri said he’s not moved by the case of one worker disappointed with her care, given that patients “die in the best hospitals … all the time.”
Workers’ compensation court records show that Heidary’s clinic dropped claims in May for payment in Rivera’s case. Attorneys involved in the case say the bills were resolved in a confidential settlement.
Workers struggle physically and legally
State and federal prosecutors have filed cases against more than 80 people for medical scams victimizing injured workers since 2010. The cases are moving forward in courthouses from Fresno to San Diego and are shaping up to be vigorous fights, with defendants battling every step of the way.
Parallel civil lawsuits also have emerged. They tend to pit insurers against medical providers in disputes over money.
But little is being done in any of the legal venues for injured workers who’ve been victimized.
Roger Brown’s doctor advised him to undergo back surgery in 2011 at Pacific Hospital of Long Beach, at the height of the cash-for-surgery scam. The operation did not go well, and he now relies on a caretaker to help him each day.
Credit: Annie Tritt for Reveal
Many, such as Denise Rivera, sign away their rights to future medical treatment in workers’ compensation cases. Others move forward with their lives, debilitated by medical care that left them worse off and unaware of the dynamics that shaped medical decisions.
That latter group includes Roger Brown, 59.
His back hurt badly after he was rear-ended in a car, but he still could work as a private investigator for a Riverside County law firm. He went fishing nearly every weekend and looked forward to annual deep-sea expeditions.
Brown’s doctor advised him to undergo back surgery in January 2011 at Pacific Hospital of Long Beach, where, Brown recalled, “he just felt the care was better.” That was at the height of the cash-for-surgery scam.
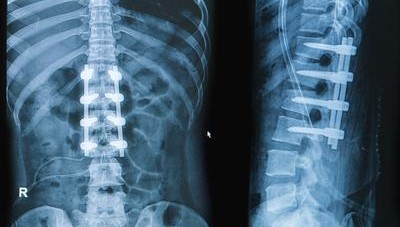
The surgery did not go well. During the first attempt to drill screws into Brown’s spine, the doctor drove special hardware 9 millimeters into his spinal cord. Even heavily medicated, the pain was unbearable.
“I would have taken my own life if I could have,” Brown said. “It was excruciating pain.”
He underwent a second surgery to fix the problem but emerged unable to drive or even work. Brown relies on a caretaker to help him each day.
In one type of fraud in the California workers’ compensation system, patients were advised to undergo high-risk surgeries by doctors who were raking in bribes.
Credit: Praisaeng/Shutterstock.com
The doctor who advised Brown to undergo the surgery in Long Beach has been accused of taking kickbacks from Michael Drobot, the executive who pleaded guilty to bribing doctors to operate at his hospital. Another surgeon who assisted in the case faces the same accusations.
Brown was so disgusted by the care that he sued for malpractice in April 2012. He didn’t get far before he decided to drop the case. As for the civil bribery accusations against his doctors, “I never heard anything like that,” Brown said.
Even if Brown had known about the illegal profiteering allegations over his medical care, it’s not clear that it would have gotten him anywhere.
Workers who’ve sustained medical harm under workers’ comp have little recourse, according to Irvine attorney Kevin Liebeck, partly because there is so little money in it for patients or lawyers.
Lawyers are reluctant to take medical malpractice cases due to caps on payouts in place since the 1970s, said Liebeck, a partner in a firm that takes such cases. Attorneys who want to help workers also are unlikely to go after a doctor for fraud because doctors’ liability insurance usually does not cover fraudulent care.
And most lawyers, he said, know that means they’ll be left struggling to get money from a doctor who can easily hide it.
“If you do stuff that is beyond the pale … and make a lot of money on it, even if you get caught and get a lot of grief, you will ultimately get out ahead,” Liebeck said. “Crime does pay for a lot of this stuff.”
Cases move forward for high-profile defendants
Whether coming out ahead is the case for some of the high-profile defendants in workers’ compensation fraud cases remains to be seen.
Drobot, the Long Beach hospital executive, faces sentencing in June for paying bribes to pack his surgery suites with workers. He also pleaded guilty to bribing former state Sen. Ronald Calderon, who is fighting accusations in a separate case for delaying legislation that cut into the astronomical profit Drobot and others made on spinal surgery hardware. Drobot declined to comment.
Cyrus Sorat, the pain-cream businessman who made the audio recording of his friend Kareem Ahmed, went to prison in 2013 following his stint as a confidential witness for prosecutors. The judge who sentenced Sorat described his undercover work as active and significant, saying it would be valuable in multiple cases.
RELATED
How California’s health care system for workers forgot about fraud
Although he faced a possible sentence of up to six and a half years, Sorat ultimately served two years in federal prison in California for mail fraud. He pleaded guilty to selling worthless billing rights to a third-party firm for pain creams that never were delivered to workers.
Sorat now faces new insurance fraud charges, also over his pain cream business. He has pleaded not guilty in the case, and his attorney did not return calls seeking comment.
Ahmed is fighting the case prosecutors filed against him in 2014. His attorney, Benjamin Gluck, said their early success in throwing out most of Ahmed’s indictment speaks “loudly about the quality of the allegations and, needless to say, we emphatically dispute them.”
Gluck noted that the undercover tapes obtained by Reveal contain no incriminating statements by Ahmed.
From what Ahmed told Sorat in their freewheeling conversation in 2010, criminal charges were not a fate he expected. Ahmed confided then that he had a plan for his millions. He wanted to build a children’s hospital in San Bernardino County – a Cedars-Sinai for kids. But, he lamented, “nobody believes me.”
Ahmed faces another legal challenge. Priscilla Lujan filed a civil lawsuit against Ahmed and her doctor in 2013. Lujan declined to be interviewed for this article, but a transcript in Ahmed’s criminal case details the hours of Andrew’s death and all that her encounter with Ahmed’s company cost her.
After losing her baby, she testified, Ahmed’s companies kept sending the pain cream to her home and billing insurers for them – $33,000 in all. She threw the boxes in her garage. She also lost custody of her older son. Child welfare officials declared her home unsafe, she said, because they believed she fed the toxic cream to her baby.
Holes in oversight leave California workers’ comp vulnerable to fraud
https://www.revealnews.org/…/holes-in-oversight-leave-cali…/
Topics: Health Care / Health Care Scams
By Christina Jewett / April 4, 2016
i
In many ways, scamming the health system meant to heal California’s injured workers is just too easy.
Anyone can hang out a shingle and purport to be a medical vendor or caregiver by sending a letter to the state – no proof required. Unscrupulous providers can run up tens of thousands of dollars in bills for meaningless drug tests, salves and medical equipment, knowing that injured workers never will lay eyes on the bill.
The gaps in oversight are so tempting that one prosecutor says scammers test-drive ways to fleece the system, often pocketing millions before anyone in a vast market of insurers catches on.
“They study the weaknesses of the system and exploit it,” said Shaddi Kamiabipour, an Orange County deputy district attorney.
Kamiabipour is among the legion of state and federal prosecutors throughout California who maintain that more than $1 billion has been siphoned out of the system.
Yet their case documents reveal something else: gaping holes in the state’s strategy to prevent fraud. The architects of other major health programs shored up similar weaknesses long ago. Here is a comparison:
Consolidate the power
When Medicare makes rules, it has a strong incentive to encourage doctors, pharmacists and others to follow them: money.
The purs
“When everyone is responsible, no one is,” said Kate Zimmermann, a Kern County prosecutor who has combated workers’ compensation fraud for eight years. “He who has the gold can write the rules. … If you have one checkbook, you can say, ‘If you want the check, this is how.’ ”
Leveraging the power to zip the wallet, the federal Affordable Care Act handed a particularly powerful fraud-fighting tool to state Medicaid agencies. They must stop paying a health care provider if they determine there is a “credible allegation of fraud.” Medical providers then can fight the determination in administrative courts.
No such rule exists in California’s workers’ compensation program. Yet the facts outlined in one case suggest it could have spared numerous questionable surgeries.
Dr. Douglas Mills testified in court that in 2007, he formally complained about a clinic at which he saw an improbable number of MRI reports come back supporting the case for surgery.
“In my opinion, people were getting hurt, so I wanted to stop it,” Mills said of his experience at San Fernando-based Frontline Medical Associates. Court records show that a state insurance department investigation was underway even before Mills’ report.
Further testimony confirmed Mills’ suspicions, including a clinic staff member who said she was paid a bonus to falsify MRI reports, bolstering the case for surgery. The revelations came to light last year – eight years after Mills’ initial complaint – when 15 people related to the clinic werecriminally indicted. The charges in the pending case include aggravated mayhem for surgeries that prosecutors deemed inappropriate.
Root out sham facilities
Medicare officials know scammers can be brazen enough to steal patient identities, fabricate a sham medical office and bill for phantom care. As a result, the federal program has set up a system to check on medical offices.
Medicare uses its own data to determine whether classes of providers with track records of graft are medium or high risk, such as wheelchair merchants and home health agencies.
Both types of providers are visited when they initially open, three or five years later – depending on the industry – and whenever officials get a complaint. A government-contracted auditor interviews operators and takes a look behind the counter, according to Jason Weinstock, a former supervisory investigator for the U.S. Health and Human Services Department’s inspector general.
In California’s workers’ compensation system, no such data reviews or facility vetting occur on a regular basis. In fact, no central authority performs inspections to make sure medical firms are doing what they claim to do.
Insurers can steer workers to a network of hand-picked medical providers. But a shadow system operates to the side, in which workers can get medical care from thousands of unregulated providers who seek payment later in workers’ compensation courts.
In that vacuum of oversight, James Allen Wilson saw a golden opportunity.
Wilson worked in the billing department at a hospital, where he had access to the personal information of workers’ compensation patients. Using their information, he set up a fake lab, billed for bogus services and started collecting $354,000 in checks at a post office box.
He got caught, according to news reports, when a savvy claims adjuster noted that he billed to perform tests on a dead man.
Wilson pleaded guilty to identity theft, grand theft and insurance fraud in 2009. In the years since, no checks of workers’ compensation medical providers have been instituted.
Empower workers to identify bogus bills
Kim Reeder of Sherman Oaks, Calif., requested a copy of her workers’ compensation medical records and discovered bills for transportation and language-interpreting services she never used.
Credit: Christina Jewett/Reveal
Albert MacKenzie, a former Los Angeles County prosecutor familiar with the Wilson case, said the oversight gaps are compounded by the fact that workers don’t have a way to flag bogus care. Unlike in Medicare or employer-paid health care, injured-worker patients aren’t mailed an explanation of benefits, or a summary of the services and charges related to their health care.
“When you have a system that doesn’t even send a patient a copy of what’s being billed for, it’s just Dodge City; open season for fraud,” MacKenzie said. “It’s just a massive cesspool.”
Kim Reeder, a worker who requested her medical records and discovered bills for transportation and language-interpreting services she never used, said mailing such information to workers would be beneficial.
“I’d like to see all workers have their billing,” said Reeder, of Sherman Oaks. “If that happens, all this can go away. I just think California is made of significantly more honest people than dishonest people.”
State labor officials say they’ve tried to clamp down on the unregulated care through legislation that gives insurers the power to deny payment for unapproved health treatments. Despite the law, though, such bills for unapproved care remain commonplace in the state’s small workers’ compensation courts.
Ban providers convicted of fraud
In Medicare, medical professionals may be banned from seeking money to see patients if they’ve been convicted of defrauding a health care program or fraud-related offenses.
But those banned providers have no problem starting a second career in California’s workers’ compensation system.
Medicare banned Dr. Thomas Heric in 2006 after he pleaded guilty to charges related to writing reports based on diagnostic tests that turned out to be fraudulent. In his letter to the judge who sentenced him, Heric pledged that going forward, he would use “whatever talents I may have in service to the community.”
Heric then found a new line of work in the workers’ compensation medical system. His job was to review data on injured workers’ sleep patterns and issue reports needed to bill insurers.
Five years later, prosecutors accused Heric of fraud again. They say he was writing virtually identical reports that gave rise to sham billing. One expert testified in court that Heric’s sleep-study reports were so bad that they failed to address one worker’s serious breathing problems for months, a lapse that he said could harm “the general public.”
That case is pending in Orange County Superior Court. Heric’s attorney, Robert Moest, said Heric stands by the reports and is fighting the charges.
“There are different opinions in the scientific community,” Moest said. “It shouldn’t be the matter of a criminal charge.”
A Reveal analysis of public records found that several other chiropractors and doctors banned by Medicare moved their career to workers’ compensation.
Among them: chiropractor David C. Nguyen. Medicare banned him in 2005 over an insurance fraud conviction. Earlier this year, San Diego prosecutors indicted him for insurance fraud again, this time for passing along bribes from a chiropractor to a therapy center – both workers’ compensation medical providers.
Look at who’s running the place
Medicare doesn’t bar just doctors, pharmacists and chiropractors with histories of fraud. It also takes a look at who’s in charge.
Officials with the Department of Health and Human Services’ inspector general’s office will investigate clinic operators’ ownership and ban those with a 5 percent or greater stake who have a history of certain fraud convictions, according to Jason Weinstock. The rule covers direct and indirect ownership.
No such rule exists in workers’ comp. State labor department officials said they do not have the authority to review the practices of medical professionals.
Instead, they said in a statement, the boards that issue licenses to medical providers are the “appropriate authority for regulation and review.” Yet no board or commission checks who’s running workers’ compensation clinics.
The state’s chiropractic board stripped Fred Khalili of his license anddenied his attempt to get it back in 2013. But he still signs physicians’ paychecks at two Los Angeles County workers’ compensation clinics.
Khalili’s legal problems started in 1995, when an FBI agent informed him that he was under investigation for paying $135,000 in kickbacks to auto-injury lawyers. Khalili was seeing a steady flow of patients who’d been hurt in car crashes, court records say.
Facing an indictment, he began to work undercover for the FBI. He recorded phone conversations with lawyers who demanded a cut of his medical treatment income in exchange for a parade of patients. He even went to the office of one lawyer who was believed to be a member of a Russian gang and kept a gun in his desk drawer, according to court records.
Khalili ultimately pleaded guilty to wire fraud and tax evasion and lost his chiropractic license in 2000. Twelve years later, he returned to the chiropractic board, hoping to get his license reinstated. The board refused, citing subsequent arrests for vandalism, a hit-and-run collision, driving without a license and making harassing phone calls. He appealed the decision to a higher court but lost.
Khalili remains heavily involved in workers’ compensation clinics, something that would draw scrutiny under Medicare’s rules as a fraud prevention measure. In the vacuum of such oversight in workers’ compensation, prosecutors now are pursuing charges against Khalili.
He was accused in February of insurance fraud for accepting kickbacks on behalf of First Choice Healthcare Medical Group clinics in Los Angeles and Panorama City. In exchange for the kickbacks, he directed staff at the clinics to dispense expensive pain creams to injured workers, the case alleges.
The charges against Khalili say he directed an attorney in 2009 to put the clinic ownership in the name of a physician, but Khalili controls the bank accounts. Attorney Malcolm McNeil, who advises First Choice, said Khalili does not own the clinics.
Khalili has not entered a plea in the case, and his criminal attorney did not return calls for comment.
Free the data
Frank Neuhauser, a UC Berkeley researcher who’s studied the California workers’ compensation system for 25 years, says opening up billing data would be politically difficult.
Credit: UC Berkeley Institute for the Study of Societal Issues
Last summer, Medicare released millions of records detailing the services and charges of doctors across the nation. The federal agency billed it as a move “to promote better care, smarter spending, and healthier people.”
The Medicare data identifies doctors’ billing practices down to the specifictest or treatment.
A flood of news stories based on the data followed, identifying high-billing doctors who also were in the crosshairs of law enforcement.
Among them was a Florida physicianaccused in a Justice Department lawsuit of performing invasive procedures to clean out seniors’ arteries – even if they didn’t need it. Another top biller is accused of reaping millions for diagnosing seniors with an eye malady that leads to blindness, whether or not they had the ailment.
No such transparency effort sheds light on health care spending in California’s workers’ compensation program. Public records in workers’ comp cases are limited to the names of medical providers seeking money in contested court cases.
Barbara Wynn, a Rand Corp. expert who was commissioned by the state to study health spending in its workers’ comp program, has access to the data as a researcher. She said making it available to the public could deter questionable practices: “It could start fingering potential fraud situations.”
Yet the data she has seen is riddled with gaps, she said. She said rules that allow the state to fine insurers that fail to report data are seldom enforced.
“If you’re going to profile what’s happening, you’re only looking at half a deck,” Wynn said. She added that California labor department officials “have sanction authorities, and they need to exercise it. Texas does, Florida does; they really come down on it.”
California labor officials estimated that about 20 percent of the billing data is missing but said they are writing letters and following up with insurers to encourage them to report all required data.
Similar data is used in Medicare to identify aberrations and notify doctors when their treatment practices appear unusual. It’s the kind of notice that two California physicians who ended up testifying in a fraud proceeding could have used.
Dr. Javier Torres testified that in his 17 years of performing nerve tests on patients, he never did a “single fiber” nerve test.
That testimony came in a 2014 fraud case. Orange County prosecutors claim physician Sim Hoffman’s office billed for more than $9 million worth of “single fiber EMG” tests that it was not even equipped to perform.
During the test, a hair-thin needle is dipped into a muscle to detect the nerve jitters that are the hallmark of a disease called myasthenia gravis, which causes weakness and difficulty breathing. It’s believed to be a disease you’re born with – not something you pick up at work or from doing heavy labor.
That didn’t stop Hoffman’s office from billing for 18 such procedures in Torres’ name, for a total of more than $8,000, according to court testimony. Hoffman has pleaded not guilty to insurance fraud, and his attorney said in a court filing that the charges against him are so vague and voluminous that “he has no meaningful way to mount an adequate defense.”
Opening up billing data would be politically difficult, said Frank Neuhauser, a UC Berkeley researcher who’s studied the California workers’ compensation system for 25 years. Some doctors and attorneys for injured workers could see their income fall if excessive care is reined in.
But for workers who get questionable surgeries or treatments, and for employers who foot the bill, he said, it would be the right thing to do.
How California’s health care system for workers forgot about fraud
https://www.revealnews.org/…/how-californias-health-care-s…/
Topics: Health Care / Health Care Scams
By Christina Jewett / March 31, 2016
i
The history of fraud in the California medical system meant to help injured workers goes back decades. And there are strong signs that the latest wave of criminal prosecutions might not mark the final chapter.
RELATED
Profiteering masquerades as medical care for injured California workers
The 102-year-old system is built on a simple bargain. Workers give up the right to sue for injuries sustained on the job. In exchange, about 15 million people covered by workers’ compensation insurance in California expect access to free and readily available medical care.
State officials focused on delivering care to workers neglected to build safeguards into the system, according to Dale Banda, a former head of enforcement for the California Department of Insurance.
“You’re dealing with a program that was designed from the beginning not to incorporate fraud as a component,” he said.
It took nearly 80 years for lawmakers to establish the California Department of Insurance’s Fraud Assessment Commission, which collects money from workers’ compensation insurers and distributes it to prosecutors who press the cases.
That was 1991. By then, the system had developed a culture of corruption.
The fraud was so blatant in 1993 that James Little, then president of a workers’ compensation insurance firm, worked with a colleague to pitch the story to television outlets.
“Primetime Live” wound up capturing footage of “cappers,” people paid to recruit patients. They trolled unemployment lines trying to lure laid-off workers to clinics. Journalists put hidden cameras in a fake workers’ comp clinic and recorded jockeying for kickbacks in exchange for patient referrals.
In 1993, “Primetime Live” recorded “cappers,” people paid to recruit patients for workers’ compensation clinics. The practice is illegal.
Credit: Primetime Live
The sham clinic’s leader, using the pseudonym Paul Morgan, confessed on camera that he wanted to help clean up the system – having participated in a half-billion dollars’ worth of fraud.
He recalled that when he was in business, recruiters brought his clinic so many uninjured workers that “we would be surprised and really didn’t know what to do with a person who came through with a legitimate injury.”
Little recalls the era: “It was way out of control.”
And it seemed to get even worse. The system costs more than doubled from $9.5 billion in 1995 to $25 billion in 2002.
In 2004, a state audit found across-the-board shortcomings in state officials’ efforts to measure and investigate workers’ compensation fraud.
That was when the new governor, Arnold Schwarzenegger, aimed his star power squarely at the problem of soaring workers’ compensation costs. He swept through Costco warehouse stores from Burbank to Sacramento with TV cameras trailing him, warning that the problem could force companies out of state.
Schwarzenegger brokered a reform deal with lawmakers that brought down costs, but it is difficult to tell whether it had an impact on fraud as well. State government leaders responsible for workers’ compensation long have struggled to measure the medical fraud problem.
The state’s Department of Insurance commissioned a 2008 study, which concluded that the state’s employers were footing the bill for up to $1.3 billion a year in erroneous payments. The report dealt with errors instead of fraud, it said, because identifying fraud would mean proving criminal intentions.
The overall “error rate” was about twice the current rate in Medicare and Medicaid.
Malcolm Sparrow, a Harvard University management professor, created the method that California officials used to reach the conclusions. He said in an interview that government officials must be willing to measure fraud to control it – and then make key changes. The next step, he said, is to conduct a follow-up study to see whether the errors are falling off.
“It takes a high degree of political courage to do a measurement program rigorously,” Sparrow said. “You have to be prepared to deal with the huge embarrassment” of failure.
RATHER LISTEN TO THE STORY?
Subscribe to the Reveal podcast to get this and other stories.
California officials never followed up using the same measurement, leaving no way to determine whether they have succeeded at reducing errors. Instead, the Department of Industrial Relations commissioned a study, unveiled last year, that used different methods to examine medical spending in workers’ compensation.
That study still found problems. Even though workers were not getting hurt worse or more often on the job, medical costs had climbed $1.6 billion from 2007 to 2012.
Barbara Wynn, a researcher with the Rand Corp., led that second study. Her preliminary findings suggest one significant cost driver was the overuse of MRI studies, particularly in Southern California. The MRIs, she said, often were done too early in the course of medical treatment to be clearly medically necessary.
Wynn’s discovery raises the specter that some of those MRIs might have been part of a scam to drum up business.
Indictments unsealed in January show that two firms specializing in MRIs were part of kickback schemes meant to guarantee a steady stream of patients. Since 2007, those MRI firms have billed insurers more than $260 million for services and filed more than 50,000 demands for payment, according to a Reveal analysis of state data.
Charges in that kickback case – dubbed “Operation Backlash” – mostly cover the years since 2012, when lawmakers passed another reform package. The new law added layers of medical review over doctors’ requests for treatment. It also took aim at middlemen who collect money on behalf of medical providers.
Recent cases in an FBI-led sting suggest that despite the legal changes, fraud continues to flourish. A San Diego prosecutor who handled one part of that case said it is merely a “small constellation in a universe of workers’ comp fraud.”
“This happens all over California,” said Pedro Bernal, the San Diego County deputy district attorney. “This is how it’s done.”
Remember The Dead And Fight For The Living
Defend Our Health & Safety Rights And Our Lives And Families
Thursday April 28, 2016 7:00PM
ILWU Local 34 (next to AT&T Ballpark
801 2nd St. San Francisco, California
April 28 is Workers Memorial Day and is commemorated throughout the world for workers who have died or been injured on the job and to fight for health and safety on the job for workers and the public.
In California workers die nearly every day because of the lack of health and safety protection and many are sickened by toxins and workplace bullying on the job which is reaching epidemic rates.
There also have been incidents of =93hanging nooses=94 put up on worksites at SF Recology and the Bay Bridge to terrorize and intimidate African American and other workers.
At the same time there are only 200 Cal OSHA health and safety
inspectors for 18.5 million workers in the State and only 2,000 for the federal government. We need to demand that there be proper enforcement for health and safety violations including jail for deaths caused by violating health and safety laws.
Additionally as a result of deregulation of workers compensation in California under SB 899 and SB 863 seriously injured workers have to go through hoops and a system called independent medical review to get medical treatment and the insurance controlled Workers Comp system stalls treatment and instead doctors in many cases are forced to
prescribe opiate drugs that end up addicting injured workers and
destroying their lives.
Under Federal and California law, workers union and unorganized are supposed to be protected when they complain to OSHA about health and safety violations. The reality is that companies and bosses regularly
bully, harass and fire workers who fight for their health and safety for themselves and the public.
Federal OSHA lawyer Darrell Whitman who was investigating retaliation complaints at PG&E, Fed Ex, Test America, Lockheed Martin and other companies found that there was illegal retaliation and then OSHA management with the backing of DOL Secretary Of Labor Tom Perez. OSHA managers bullied and harassed AFGE investigators and lawyers in the Whistleblower Protection Program and illegally fired Whitman for trying to defend OSHA whistleblowers. We will discuss what workers can do to protect their rights and get justice and accountability.
It is time to remember the dead and fight for the living. We have a
right to work in a healthy and safe workplace for ourselves and our
families.
Initial Speakers:
Brenda Barros, SEIU 1021 SF General Hospital Chapter Chair
Dr. Larry Rose, Past Medical Director of Cal-OSHA
Daryle Washington, IBT 350 Worker At SF Recology
Daniel Berman, Health and Safety Advocate and author of =93Death on the Job
Dorian Maxwell, Fired MTA TWU 250A bus driver and OSHA whistleblower
Roland Sheppard, Retired Painters Local 4 BA
For more information Injured Workers National Network
http://www.iwnn.org
Endorsed by
SMART UTU 1741, IWNN, UPWA
https://www.facebook.com/Injured-Workers-National-Network-=85/
(415)282-1908
info [at] iwnn.org
Billion Dollar Scam In California Workers Comp System Destroys Workers And Bilks The Public
https://www.revealnews.org/episodes/billion-dollar-scam/
Apr 2, 2016 SHARE
California’s workers’ compensation program covers 15 million workers across the state. If you get hurt on the job – fall off a ladder, for instance – it’s the system you turn to. Most employers are required to carry workers’ comp insurance, which helps cover medical bills and lost wages for injured employees.
But Reveal reporter Christina Jewett has discovered serious fraud in the system after reviewing thousands of documents. They show that in the last decade, more than 80 people have been accused of cheating California’s workers’ comp medical system out of $1 billion.
Jewett and producer Delaney Hall tell the story using an undercover law enforcement wiretap and the accounts of a worker, employer and investigator.
Host Al Letson then sits down with Jewett to really dig into what it is that makes workers’ comp such an easy target for people who want to take advantage of it.
And finally, we revisit a story about the bogus screws that ended up in spines of surgery patients. You can consider it the prequel to the main investigation …
Profiteering masquerades as medical care for injured California workers
https://www.revealnews.org/…/profiteering-masquerades-as-m…/
By Christina Jewett / March 31, 2016
Priscilla Lujan was awake soothing her infant son at 10 p.m. and again in the middle of the night. She let him gum one of the salty pistachios she was eating. She mixed a bottle of formula at the side of their shared bed.
It was the fitful kind of night that’s easily forgotten after a strong cup of coffee and a shy smile from a sleep-refreshed baby.
But that’s not what happened the next morning. When Lujan woke up, her son – not yet 6 months old on Feb. 3, 2012 – was cold. His lips, blue. His eyes, half open. She screamed to her mother to call 911.
At the hospital, Lujan stood in a room rocking her baby from side to side, sobbing. By then, Andrew Gallegos already was dead.
Police showed up at Lujan’s East Los Angeles home about a week later – more than a dozen of them. They seized her medications. They handcuffed her and drove her to the police station, where a detective demanded answers: Why did her baby have toxic levels of pain medicine in his bloodstream?
During the interview, it dawned on Lujan: The pain cream she had slathered on her knee had gotten into her son’s mouth, through the pistachio and bottle of formula.
Photos of tubes of pain cream seized from Priscilla Lujan’s home were presented to an Orange County grand jury. Prosecutors alleged that businessman Kareem Ahmed helped formulate the toxic cream and was culpable in the death of Lujan’s infant son.
Credit: Orange County Superior Court
“Oh my God, I killed my baby,” she told the detective.
Soon after, the focus of the case shifted. The new target was Kareem Ahmed, a millionaire businessman who made his fortune selling medicated creams for patients like Lujan, who struggled with pain after an injury on the job.
Ahmed eventually would be indicted for involuntary manslaughter in Andrew’s death and accused of a far more sweeping crime: paying more than $25 million in bribes to doctors, including Lujan’s, who prescribed the pain-relief creams.
To the people who combat fraud in California’s $24 billion workers’ compensation system, the case exemplifies unchecked profiteering that jeopardizes injured workers’ health and lives.
It is one of more than a dozen cases that, taken together, outline a medical landscape in which corruption masquerades as medical care for some of California’s injured workers.
A review of thousands of criminal court records by Reveal from The Center for Investigative Reporting shows a system in which pay-to-play schemes trump patient care, particularly in unregulated treatments rejected by insurers and disputed in obscure courts throughout the state.
Prosecutors are beginning to turn the tide, pursuing charges against more than 80 medical professionals who’ve handled more than 100,000 injured-worker cases, most of them originating in Southern California.
Defendants include a physician assistant accused of “aggravated mayhem” after he operated on dozens of injured workers’ knees and shoulders, despite lacking surgical training. The outcomes often were disastrous.
“It still hurts today,” one worker testified in 2015, describing his unsuccessful 2010 shoulder surgery through an interpreter. “I can’t, you know, bend my arm, really.”
Along with the court records, Reveal analyzed data from more than a million workers’ compensation court cases, which show that over the last decade, workers have been swept into medical billing mills, prescribed unregulated medications and advised to undergo sometimes unneeded or high-risk surgery by doctors who were raking in bribes.
RATHER LISTEN TO THE STORY?
Subscribe to the Reveal podcast to get this and other stories.
Prosecutors estimate that the accused have burdened the system with more than $1 billion in demands for money intended to help injured workers get back on the job.
The cases are being fought vigorously at every turn. Ahmed’s attorney secured an early victory, getting all but one count in his indictment thrown out; the prosecutor says she will refile the charges. Other attorneys defending the accused say the barrage of cases is a witch hunt that scares medical providers away from the system, limiting workers’ access to care.
Taken together, the alleged schemes inject cynicism into a system in which workers already are at odds with insurers, which can save money when they deny care. They heap costs in the form of higher premiums on employers, who in turn raise prices for goods or services or stem hiring as they pay the highest workers’ compensation rates in the nation.
Workers such as Tammy Martinez, though, pay the greatest price. The 56-year-old truck driver hurt her back pushing a 1-ton cart.
The workers’ compensation attorney whom she relied on to help her navigate the system pleaded guilty in 2014 to being part of a criminal club: people taking bribes from hospital executive Michael Drobot.
Drobot had pleaded guilty in early 2014 to paying at least $20 million in kickbacks to dozens of marketers, doctors and others who helped him fill the surgery suites at the now-defunct Pacific Hospital of Long Beach. Federal prosecutors linked the bribes to more than 4,400 risky spinal operations at the hospital.
Martinez’s lawyer, Sean O’Keefe, recommended that she see a surgeon, who, she later would learn, also was accused of taking bribes from Drobot. O’Keefe’s guilty plea singles out Martinez’s case as one spurred by illegal bribes and a conspiracy compelling her surgeon to perform a particularly complex – and expensive – operation.
Michael Drobot, executive of the now-defunct Pacific Hospital of Long Beach, pleaded guilty in 2014 to paying at least $20 million in bribes to bring spinal surgeries to his hospital.
Credit: Pacific Hospital of Long Beach website via Archive.org
When it came time for Martinez’s spinal surgery in October 2011, all did not go well. Doctors noted that after the procedure, her left foot grew pale and pulseless. Within weeks, her leg had to be amputated above the knee.
Since then, she said, it’s been a difficult journey to learn to stand again and to discover that her young grandson was not, in fact, afraid of her.
“I lost myself,” Martinez said. “I struggle every day to get the person I used to be back.”
Across Southern California, Reveal found, companies employ intensive marketing to tap into a particularly vulnerable segment of the workforce. They blanket Spanish-language media with ads and target Latinos with calls to their homes. They suggest that filing a case could lead to a windfall.
“Receive up to $4,000 per month,” proclaim Spanish-language signs, business cards and fliers posted across Southern California. One workers’ compensation attorney troubled by the ads called the number out of curiosity. After that, messages from a buzzing call center lit up his phone five times a day – for months.
Callers wanted to know “if I knew anyone who had been injured,” San Diego attorney John A. Don said, “if I could refer anyone to them.”
Christine Baker, director of the state Department of Industrial Relations, which administers workers’ compensation, initially responded to questions with a statement noting that other state authorities oversee medical providers and health fraud. But two weeks ago, she said her department had taken a closer look at unregulated medical care, and “we know there’s a problem.”
“We want workers to get appropriate care,” she said. “We don’t want overcare or undercare; either way is wrong. Delivery of care needs to be evidence-based, appropriate and quickly delivered.”
Baker said medical abuse is a symptom of a “deeper problem,” particularly in Southern California.
There, workers’ comp stands out as an easy target for scammers. While health care programs such as Medicare have developed an arsenal of weapons to ward off fraud, California state regulators have few tools at their disposal. For one thing, the state shares oversight with hundreds of insurers and self-insured employers, leaving no one clearly in charge.
Prosecutors filing a growing parade of cases are exposing this leadership vacuum and how it allows operatives to bypass the most competent medical providers for the highest bidder. Workers who’ve been hurt on the job often are the last to find out that they have been exploited – if they find out at all.
“We’re talking about a patient that has become a commodity,” said Don Marshall, chairman of the state’s Fraud Assessment Commission, which distributes funds to prosecutors who fight workers’ compensation fraud. “It’s become something to trade and sell on the open market for no other reason than to generate income.”
‘Nobody cares’ about workers’ comp
As investigators began to puzzle over the 2012 death of Andrew Gallegos, it did not take them long to realize they already had a window into the world of the man who ultimately would be charged in the case.
Businessman Kareem Ahmed has been accused of paying more than $25 million in kickbacks to doctors in a workers’ compensation fraud scheme.
Credit: Paul A. Hebert/Invision/AP file
Kareem Ahmed was the owner of Landmark Medical Management. He is not a pharmacist. But prosecutors, in the continuing legal case against him related to Andrew’s death, would point out that he still delved into the science of mixing medications to formulate pain creams.
Ahmed’s goal, they allege, was not to make the most effective salve, but the most profitable one. Experts would testify that, if ingested, the opioid-infused cream was a “loaded gun” that could kill an adult. His firms billed insurers $400 to $1,700 per tube for creams sent to Priscilla Lujan, totaling $59,000, court records show.
An undercover recording made nearly four years before Ahmed’s indictment gives a wider view of the world of workers’ compensation medical executives. In that recording, Ahmed makes it clear that many of them are up to no good – and no one is stopping them.
Businessman Cyrus Sorat secretly recorded the conversation. Also in the pain cream business, Sorat was working for federal prosecutors as part of an agreement to seek leniency in a separate workers’ compensation fraud case.
As the two men shared a leisurely lunch at an upscale restaurant in Ontario, California, Ahmed marveled over the scale of the exploits of others who, like him, made their millions off health care for injured workers.
One stood out, he said, for paying doctors up to $50,000 a month to perform invasive and risky back surgeries: Drobot, the Long Beach hospital executive who eventually would plead guilty to bribing the surgeons.
“How come nobody does anything to him, man?” Ahmed implores in the recording, pounding the table.
When it comes to workers’ comp, nobody cares.”
— Kareem Ahmed
owner of Landmark Medical Management, in a secretly recorded conversation with businessman Cyrus Sorat
Sorat lowers his voice. “Let me tell you something. If you do Medicare – the feds hang you,” he says.
“Oh, I know, that’s why I never touch Medicare,” Ahmed says.
“But when it comes to workers’ comp, …” Sorat continues.
“Nobody gives a fuck,” Ahmed finishes the sentence.
“Nobody cares,” Sorat agrees. Ahmed laughs.
The men go on to discuss other workers’ compensation moguls. They cluck about a former chiropractor who they say had gotten a multimillion-dollar settlement from a large insurer. Sorat calls him “a criminal.”
SIGN UP FOR OUR NEWSLETTER
Stay up to date with the latest investigations and episodes from Reveal delivered to your inbox.
“Yeah, and then he gets money. He’s wanted in six different states,” Ahmed said. “But nobody did anything. … Nobody does shit.”
They also talk about David Wayne Fish, a businessman who pleaded no contest in 2010 to taking money for patient referrals. He was accused of organizing dozens of lawyers and doctors to steer more than 4,000 cases to preferred medical providers and run up high bills.
Fish’s sentence: probation, fines and an order to stop demanding the $60 million he was seeking from insurers.
“He’s … walking! What happened to him? Nothing,” Ahmed said. “Six fucking years of (investigation), thousands of hours, and he’s walking? … He’ll … make a $100 million in one year again.”
“When it comes to workers’ comp, …” Sorat said.
Ahmed finished his sentence once again: “Yeah, nobody cares.”
Abuse abounds in specialized courts
On a sunny Monday in November, the workers’ compensation court in Marina del Rey is swarming with activity. Lawyers weave down the halls from small courtroom to courtroom and gather in clusters. Others fervently broker deals on their cellphones.
There are 24 courts like this up and down the state. But the activity is particularly frenetic in Southern California, where the paperwork that fuels the court’s pace comes in by the virtual truckload.
Christine Baker, director of the California Department of Industrial Relations, says her department has taken a closer look at unregulated medical care, and “we know there’s a problem.”
Credit: California Department of Industrial Relations
These courts spend the bulk of their time settling liens – claims for payments that medical and other service providers file against insurers or self-insured employers.
The lien system was created to protect the injured worker. It guarantees that even if insurers deny medical care, workers will have a medical professional to whom they can turn.
But the system also throws its doors open to providers excluded from insurers’ networks of preferred professionals. It allows thousands of unregulated entities to bill for any treatment, whiz-bang device, pain cream or DNA test. The only limit is the providers’ willingness to roll the dice on how much money they’ll rake in at workers’ comp courts.
The lien system thrives in California – more than in any other state. One national insurance executive estimated in 2010 that his company does one-fifth of its business in California – but deals with more than four-fifths of its liens there.
That volume creates “a very thick forest for thieves and scoundrels to hide out in,” said Lachlan Taylor, a former special counsel to the Department of Industrial Relations who analyzed the lien system in 2010.
His work informed a 2012 law that cut down on liens with a new $150 fee required to demand payment in workers’ compensation courts. It also gave insurers new powers to deny money to providers that aren’t approved to treat injured workers.
Yet claims for unapproved care still are cropping up, said Baker, the Department of Industrial Relations’ chief. And the number of liens filed last year is even higher than it was when Taylor initially concluded that the system “rewards bad behavior.”
Baker said her department has begun reviewing the medical providers who currently file the largest number of liens. The result: “We do note that many are (criminally) indicted.”
The shifting array of schemes is difficult for government authorities to track, much less for workers such as Denise Rivera. Her medical care providers amassed bills – or liens – amounting to $95,000. Yet the knee she sought help with continues to ache, swell and give out.
She injured it while working at a center for severely disabled children, a nursing assistant job she loved. She worked the night shift, feeding children, turning them when they slept and getting them ready for the next day.
“When you came in, (the kids) had a smile for you,” said Rivera, who lives in Riverside County.
Two days after Thanksgiving in 2011, she slipped and fell while giving a child a shower. Rivera said she immediately felt paralyzed by leg and back pain. Her company’s doctor said she needed knee surgery, but her employer’s insurance company denied the request.
Rivera saw a commercial on TV for legal help with a work-injury case, called the number and got connected to California Injury Lawyer Inc. The Corona-based company sent people to her house to take her information and referred her to a Riverside clinic, she said.
They’re intrusive. I have people tell me that they’ll call every single day.”
— Teena Barton
ICW Group Insurance Cos. special investigator, on marketers and advertisers
Teena Barton is familiar with this kind of advertising through her work as a special investigator in San Diego for the ICW Group Insurance Cos., a workers’ compensation insurance firm.
Barton said marketers and advertisers are invasive, often pressuring workers to refer friends and co-workers, who get cold calls at home. She said workers often are pressured into filing work injury claims and put on a lengthy course of medical treatment.
“The problem is once you’re on that wave, that wave’s going to take you,” Barton said. “That’s what the system is. ”
Multiple medical procedures
The people who asked Denise Rivera, 54, to sign papers advised her to report to a Riverside clinic, she said.
The clinic packed her schedule with appointments. Clinic staff gave her what looked like a school lunch menu, with the names of doctors and companies she was expected to see three times per week.
Rivera cobbled together the gas money or borrowed family members’ cars to make her appointments. She sat in the clinic’s jammed waiting room for hours at a time and watched medical staff wheel in suitcases full of devices to treat workers.
Denise Rivera said she didn’t work for four years while waiting for her workers’ compensation case to be resolved. She ultimately got a settlement for $32,500 – about a year’s pay.
Credit: John M. Blodgett for Reveal
She said she received MRIs, acupuncture, shockwave therapy and treatments with a device that seemed like a jackhammer thumping her knee. At one point, clinic staff sent her home with an electrical pain treatment device, but they forgot to include the electrode pads needed to make it work.
Pain creams that “seemed like Bengay,” according to Rivera, arrived in the mail. For those creams alone, records show that Kareem Ahmed’s company billed $17,102. Ahmed is the pain-cream executive who was charged in baby Andrew Gallegos’ death. The pharmacist who made 145,000 tubes of cream for his company got $35 to $72 per tube, public records say.
Records in Rivera’s case show the total bill sent by providers to the insurer for her care: $95,257. She had never seen that total, and it shocked her.
“No way,” she said, then added: “None of the treatments they’ve given me has helped.”
Rivera said she did not work for four years while waiting for her workers’ compensation case to be resolved. Penniless, she set up her bedroom in her mother’s garage.
She ultimately got a settlement in the case to compensate her for a permanent disability. The amount was $32,500 – about what she would have made in one year at work.
Going after ‘The Godfather’
Riverside County prosecutors now allege that Rivera walked into a clinic, with eight affiliate sites, that ran a $122 million scam.
They filed charges in July 2014 against attorney Cary Abramowitz and chiropractor Peyman Heidary. Prosecutors say in court records that Heidary is nicknamed “The Godfather” for masterminding the profit-centered medical network that Rivera encountered.
Heidary is accused of controlling medical treatment at the clinics, even though he’s not a doctor, which is a crime in California. Prosecutors say he also illegally owned and controlled law offices, even though he’s not a lawyer.
Prosecutors claim that workers came into the network via “cappers” – people paid to recruit patients – who got referrals from English- and Spanish-language 800 numbers. At Heidary’s direction, clerical staff allegedly padded the cases with additional supposedly injured body parts, according to court records.
Of the $122 million Heidary’s group sought, one document from prosecutors indicates that it had collected $18 million from insurers as of April 2015.
Rivera said the allegations were bad news for her, given that she trusted the legal and medical professionals to fight for her best interests.
“It makes me angry,” she said. “I kind of want to cry.”
Basically, I got screwed.”
— Denise Rivera
former nursing assistant
Heidary has pleaded not guilty. His attorney, Michael Khouri, said the case lacks legal and factual merit and has ruined Heidary’s reputation. All the care, he said, was medically necessary.
When told about Rivera’s plight, Khouri said he’s not moved by the case of one worker disappointed with her care, given that patients “die in the best hospitals … all the time.”
Workers’ compensation court records show that Heidary’s clinic dropped claims in May for payment in Rivera’s case. Attorneys involved in the case say the bills were resolved in a confidential settlement.
Workers struggle physically and legally
State and federal prosecutors have filed cases against more than 80 people for medical scams victimizing injured workers since 2010. The cases are moving forward in courthouses from Fresno to San Diego and are shaping up to be vigorous fights, with defendants battling every step of the way.
Parallel civil lawsuits also have emerged. They tend to pit insurers against medical providers in disputes over money.
But little is being done in any of the legal venues for injured workers who’ve been victimized.
Roger Brown’s doctor advised him to undergo back surgery in 2011 at Pacific Hospital of Long Beach, at the height of the cash-for-surgery scam. The operation did not go well, and he now relies on a caretaker to help him each day.
Credit: Annie Tritt for Reveal
Many, such as Denise Rivera, sign away their rights to future medical treatment in workers’ compensation cases. Others move forward with their lives, debilitated by medical care that left them worse off and unaware of the dynamics that shaped medical decisions.
That latter group includes Roger Brown, 59.
His back hurt badly after he was rear-ended in a car, but he still could work as a private investigator for a Riverside County law firm. He went fishing nearly every weekend and looked forward to annual deep-sea expeditions.
Brown’s doctor advised him to undergo back surgery in January 2011 at Pacific Hospital of Long Beach, where, Brown recalled, “he just felt the care was better.” That was at the height of the cash-for-surgery scam.
The surgery did not go well. During the first attempt to drill screws into Brown’s spine, the doctor drove special hardware 9 millimeters into his spinal cord. Even heavily medicated, the pain was unbearable.
“I would have taken my own life if I could have,” Brown said. “It was excruciating pain.”
He underwent a second surgery to fix the problem but emerged unable to drive or even work. Brown relies on a caretaker to help him each day.
In one type of fraud in the California workers’ compensation system, patients were advised to undergo high-risk surgeries by doctors who were raking in bribes.
Credit: Praisaeng/Shutterstock.com
The doctor who advised Brown to undergo the surgery in Long Beach has been accused of taking kickbacks from Michael Drobot, the executive who pleaded guilty to bribing doctors to operate at his hospital. Another surgeon who assisted in the case faces the same accusations.
Brown was so disgusted by the care that he sued for malpractice in April 2012. He didn’t get far before he decided to drop the case. As for the civil bribery accusations against his doctors, “I never heard anything like that,” Brown said.
Even if Brown had known about the illegal profiteering allegations over his medical care, it’s not clear that it would have gotten him anywhere.
Workers who’ve sustained medical harm under workers’ comp have little recourse, according to Irvine attorney Kevin Liebeck, partly because there is so little money in it for patients or lawyers.
Lawyers are reluctant to take medical malpractice cases due to caps on payouts in place since the 1970s, said Liebeck, a partner in a firm that takes such cases. Attorneys who want to help workers also are unlikely to go after a doctor for fraud because doctors’ liability insurance usually does not cover fraudulent care.
And most lawyers, he said, know that means they’ll be left struggling to get money from a doctor who can easily hide it.
“If you do stuff that is beyond the pale … and make a lot of money on it, even if you get caught and get a lot of grief, you will ultimately get out ahead,” Liebeck said. “Crime does pay for a lot of this stuff.”
Cases move forward for high-profile defendants
Whether coming out ahead is the case for some of the high-profile defendants in workers’ compensation fraud cases remains to be seen.
Drobot, the Long Beach hospital executive, faces sentencing in June for paying bribes to pack his surgery suites with workers. He also pleaded guilty to bribing former state Sen. Ronald Calderon, who is fighting accusations in a separate case for delaying legislation that cut into the astronomical profit Drobot and others made on spinal surgery hardware. Drobot declined to comment.
Cyrus Sorat, the pain-cream businessman who made the audio recording of his friend Kareem Ahmed, went to prison in 2013 following his stint as a confidential witness for prosecutors. The judge who sentenced Sorat described his undercover work as active and significant, saying it would be valuable in multiple cases.
RELATED
How California’s health care system for workers forgot about fraud
Although he faced a possible sentence of up to six and a half years, Sorat ultimately served two years in federal prison in California for mail fraud. He pleaded guilty to selling worthless billing rights to a third-party firm for pain creams that never were delivered to workers.
Sorat now faces new insurance fraud charges, also over his pain cream business. He has pleaded not guilty in the case, and his attorney did not return calls seeking comment.
Ahmed is fighting the case prosecutors filed against him in 2014. His attorney, Benjamin Gluck, said their early success in throwing out most of Ahmed’s indictment speaks “loudly about the quality of the allegations and, needless to say, we emphatically dispute them.”
Gluck noted that the undercover tapes obtained by Reveal contain no incriminating statements by Ahmed.
From what Ahmed told Sorat in their freewheeling conversation in 2010, criminal charges were not a fate he expected. Ahmed confided then that he had a plan for his millions. He wanted to build a children’s hospital in San Bernardino County – a Cedars-Sinai for kids. But, he lamented, “nobody believes me.”
Ahmed faces another legal challenge. Priscilla Lujan filed a civil lawsuit against Ahmed and her doctor in 2013. Lujan declined to be interviewed for this article, but a transcript in Ahmed’s criminal case details the hours of Andrew’s death and all that her encounter with Ahmed’s company cost her.
After losing her baby, she testified, Ahmed’s companies kept sending the pain cream to her home and billing insurers for them – $33,000 in all. She threw the boxes in her garage. She also lost custody of her older son. Child welfare officials declared her home unsafe, she said, because they believed she fed the toxic cream to her baby.
Holes in oversight leave California workers’ comp vulnerable to fraud
https://www.revealnews.org/…/holes-in-oversight-leave-cali…/
Topics: Health Care / Health Care Scams
By Christina Jewett / April 4, 2016
i
In many ways, scamming the health system meant to heal California’s injured workers is just too easy.
Anyone can hang out a shingle and purport to be a medical vendor or caregiver by sending a letter to the state – no proof required. Unscrupulous providers can run up tens of thousands of dollars in bills for meaningless drug tests, salves and medical equipment, knowing that injured workers never will lay eyes on the bill.
The gaps in oversight are so tempting that one prosecutor says scammers test-drive ways to fleece the system, often pocketing millions before anyone in a vast market of insurers catches on.
“They study the weaknesses of the system and exploit it,” said Shaddi Kamiabipour, an Orange County deputy district attorney.
Kamiabipour is among the legion of state and federal prosecutors throughout California who maintain that more than $1 billion has been siphoned out of the system.
Yet their case documents reveal something else: gaping holes in the state’s strategy to prevent fraud. The architects of other major health programs shored up similar weaknesses long ago. Here is a comparison:
Consolidate the power
When Medicare makes rules, it has a strong incentive to encourage doctors, pharmacists and others to follow them: money.
The purs
“When everyone is responsible, no one is,” said Kate Zimmermann, a Kern County prosecutor who has combated workers’ compensation fraud for eight years. “He who has the gold can write the rules. … If you have one checkbook, you can say, ‘If you want the check, this is how.’ ”
Leveraging the power to zip the wallet, the federal Affordable Care Act handed a particularly powerful fraud-fighting tool to state Medicaid agencies. They must stop paying a health care provider if they determine there is a “credible allegation of fraud.” Medical providers then can fight the determination in administrative courts.
No such rule exists in California’s workers’ compensation program. Yet the facts outlined in one case suggest it could have spared numerous questionable surgeries.
Dr. Douglas Mills testified in court that in 2007, he formally complained about a clinic at which he saw an improbable number of MRI reports come back supporting the case for surgery.
“In my opinion, people were getting hurt, so I wanted to stop it,” Mills said of his experience at San Fernando-based Frontline Medical Associates. Court records show that a state insurance department investigation was underway even before Mills’ report.
Further testimony confirmed Mills’ suspicions, including a clinic staff member who said she was paid a bonus to falsify MRI reports, bolstering the case for surgery. The revelations came to light last year – eight years after Mills’ initial complaint – when 15 people related to the clinic werecriminally indicted. The charges in the pending case include aggravated mayhem for surgeries that prosecutors deemed inappropriate.
Root out sham facilities
Medicare officials know scammers can be brazen enough to steal patient identities, fabricate a sham medical office and bill for phantom care. As a result, the federal program has set up a system to check on medical offices.
Medicare uses its own data to determine whether classes of providers with track records of graft are medium or high risk, such as wheelchair merchants and home health agencies.
Both types of providers are visited when they initially open, three or five years later – depending on the industry – and whenever officials get a complaint. A government-contracted auditor interviews operators and takes a look behind the counter, according to Jason Weinstock, a former supervisory investigator for the U.S. Health and Human Services Department’s inspector general.
In California’s workers’ compensation system, no such data reviews or facility vetting occur on a regular basis. In fact, no central authority performs inspections to make sure medical firms are doing what they claim to do.
Insurers can steer workers to a network of hand-picked medical providers. But a shadow system operates to the side, in which workers can get medical care from thousands of unregulated providers who seek payment later in workers’ compensation courts.
In that vacuum of oversight, James Allen Wilson saw a golden opportunity.
Wilson worked in the billing department at a hospital, where he had access to the personal information of workers’ compensation patients. Using their information, he set up a fake lab, billed for bogus services and started collecting $354,000 in checks at a post office box.
He got caught, according to news reports, when a savvy claims adjuster noted that he billed to perform tests on a dead man.
Wilson pleaded guilty to identity theft, grand theft and insurance fraud in 2009. In the years since, no checks of workers’ compensation medical providers have been instituted.
Empower workers to identify bogus bills
Kim Reeder of Sherman Oaks, Calif., requested a copy of her workers’ compensation medical records and discovered bills for transportation and language-interpreting services she never used.
Credit: Christina Jewett/Reveal
Albert MacKenzie, a former Los Angeles County prosecutor familiar with the Wilson case, said the oversight gaps are compounded by the fact that workers don’t have a way to flag bogus care. Unlike in Medicare or employer-paid health care, injured-worker patients aren’t mailed an explanation of benefits, or a summary of the services and charges related to their health care.
“When you have a system that doesn’t even send a patient a copy of what’s being billed for, it’s just Dodge City; open season for fraud,” MacKenzie said. “It’s just a massive cesspool.”
Kim Reeder, a worker who requested her medical records and discovered bills for transportation and language-interpreting services she never used, said mailing such information to workers would be beneficial.
“I’d like to see all workers have their billing,” said Reeder, of Sherman Oaks. “If that happens, all this can go away. I just think California is made of significantly more honest people than dishonest people.”
State labor officials say they’ve tried to clamp down on the unregulated care through legislation that gives insurers the power to deny payment for unapproved health treatments. Despite the law, though, such bills for unapproved care remain commonplace in the state’s small workers’ compensation courts.
Ban providers convicted of fraud
In Medicare, medical professionals may be banned from seeking money to see patients if they’ve been convicted of defrauding a health care program or fraud-related offenses.
But those banned providers have no problem starting a second career in California’s workers’ compensation system.
Medicare banned Dr. Thomas Heric in 2006 after he pleaded guilty to charges related to writing reports based on diagnostic tests that turned out to be fraudulent. In his letter to the judge who sentenced him, Heric pledged that going forward, he would use “whatever talents I may have in service to the community.”
Heric then found a new line of work in the workers’ compensation medical system. His job was to review data on injured workers’ sleep patterns and issue reports needed to bill insurers.
Five years later, prosecutors accused Heric of fraud again. They say he was writing virtually identical reports that gave rise to sham billing. One expert testified in court that Heric’s sleep-study reports were so bad that they failed to address one worker’s serious breathing problems for months, a lapse that he said could harm “the general public.”
That case is pending in Orange County Superior Court. Heric’s attorney, Robert Moest, said Heric stands by the reports and is fighting the charges.
“There are different opinions in the scientific community,” Moest said. “It shouldn’t be the matter of a criminal charge.”
A Reveal analysis of public records found that several other chiropractors and doctors banned by Medicare moved their career to workers’ compensation.
Among them: chiropractor David C. Nguyen. Medicare banned him in 2005 over an insurance fraud conviction. Earlier this year, San Diego prosecutors indicted him for insurance fraud again, this time for passing along bribes from a chiropractor to a therapy center – both workers’ compensation medical providers.
Look at who’s running the place
Medicare doesn’t bar just doctors, pharmacists and chiropractors with histories of fraud. It also takes a look at who’s in charge.
Officials with the Department of Health and Human Services’ inspector general’s office will investigate clinic operators’ ownership and ban those with a 5 percent or greater stake who have a history of certain fraud convictions, according to Jason Weinstock. The rule covers direct and indirect ownership.
No such rule exists in workers’ comp. State labor department officials said they do not have the authority to review the practices of medical professionals.
Instead, they said in a statement, the boards that issue licenses to medical providers are the “appropriate authority for regulation and review.” Yet no board or commission checks who’s running workers’ compensation clinics.
The state’s chiropractic board stripped Fred Khalili of his license anddenied his attempt to get it back in 2013. But he still signs physicians’ paychecks at two Los Angeles County workers’ compensation clinics.
Khalili’s legal problems started in 1995, when an FBI agent informed him that he was under investigation for paying $135,000 in kickbacks to auto-injury lawyers. Khalili was seeing a steady flow of patients who’d been hurt in car crashes, court records say.
Facing an indictment, he began to work undercover for the FBI. He recorded phone conversations with lawyers who demanded a cut of his medical treatment income in exchange for a parade of patients. He even went to the office of one lawyer who was believed to be a member of a Russian gang and kept a gun in his desk drawer, according to court records.
Khalili ultimately pleaded guilty to wire fraud and tax evasion and lost his chiropractic license in 2000. Twelve years later, he returned to the chiropractic board, hoping to get his license reinstated. The board refused, citing subsequent arrests for vandalism, a hit-and-run collision, driving without a license and making harassing phone calls. He appealed the decision to a higher court but lost.
Khalili remains heavily involved in workers’ compensation clinics, something that would draw scrutiny under Medicare’s rules as a fraud prevention measure. In the vacuum of such oversight in workers’ compensation, prosecutors now are pursuing charges against Khalili.
He was accused in February of insurance fraud for accepting kickbacks on behalf of First Choice Healthcare Medical Group clinics in Los Angeles and Panorama City. In exchange for the kickbacks, he directed staff at the clinics to dispense expensive pain creams to injured workers, the case alleges.
The charges against Khalili say he directed an attorney in 2009 to put the clinic ownership in the name of a physician, but Khalili controls the bank accounts. Attorney Malcolm McNeil, who advises First Choice, said Khalili does not own the clinics.
Khalili has not entered a plea in the case, and his criminal attorney did not return calls for comment.
Free the data
Frank Neuhauser, a UC Berkeley researcher who’s studied the California workers’ compensation system for 25 years, says opening up billing data would be politically difficult.
Credit: UC Berkeley Institute for the Study of Societal Issues
Last summer, Medicare released millions of records detailing the services and charges of doctors across the nation. The federal agency billed it as a move “to promote better care, smarter spending, and healthier people.”
The Medicare data identifies doctors’ billing practices down to the specifictest or treatment.
A flood of news stories based on the data followed, identifying high-billing doctors who also were in the crosshairs of law enforcement.
Among them was a Florida physicianaccused in a Justice Department lawsuit of performing invasive procedures to clean out seniors’ arteries – even if they didn’t need it. Another top biller is accused of reaping millions for diagnosing seniors with an eye malady that leads to blindness, whether or not they had the ailment.
No such transparency effort sheds light on health care spending in California’s workers’ compensation program. Public records in workers’ comp cases are limited to the names of medical providers seeking money in contested court cases.
Barbara Wynn, a Rand Corp. expert who was commissioned by the state to study health spending in its workers’ comp program, has access to the data as a researcher. She said making it available to the public could deter questionable practices: “It could start fingering potential fraud situations.”
Yet the data she has seen is riddled with gaps, she said. She said rules that allow the state to fine insurers that fail to report data are seldom enforced.
“If you’re going to profile what’s happening, you’re only looking at half a deck,” Wynn said. She added that California labor department officials “have sanction authorities, and they need to exercise it. Texas does, Florida does; they really come down on it.”
California labor officials estimated that about 20 percent of the billing data is missing but said they are writing letters and following up with insurers to encourage them to report all required data.
Similar data is used in Medicare to identify aberrations and notify doctors when their treatment practices appear unusual. It’s the kind of notice that two California physicians who ended up testifying in a fraud proceeding could have used.
Dr. Javier Torres testified that in his 17 years of performing nerve tests on patients, he never did a “single fiber” nerve test.
That testimony came in a 2014 fraud case. Orange County prosecutors claim physician Sim Hoffman’s office billed for more than $9 million worth of “single fiber EMG” tests that it was not even equipped to perform.
During the test, a hair-thin needle is dipped into a muscle to detect the nerve jitters that are the hallmark of a disease called myasthenia gravis, which causes weakness and difficulty breathing. It’s believed to be a disease you’re born with – not something you pick up at work or from doing heavy labor.
That didn’t stop Hoffman’s office from billing for 18 such procedures in Torres’ name, for a total of more than $8,000, according to court testimony. Hoffman has pleaded not guilty to insurance fraud, and his attorney said in a court filing that the charges against him are so vague and voluminous that “he has no meaningful way to mount an adequate defense.”
Opening up billing data would be politically difficult, said Frank Neuhauser, a UC Berkeley researcher who’s studied the California workers’ compensation system for 25 years. Some doctors and attorneys for injured workers could see their income fall if excessive care is reined in.
But for workers who get questionable surgeries or treatments, and for employers who foot the bill, he said, it would be the right thing to do.
How California’s health care system for workers forgot about fraud
https://www.revealnews.org/…/how-californias-health-care-s…/
Topics: Health Care / Health Care Scams
By Christina Jewett / March 31, 2016
i
The history of fraud in the California medical system meant to help injured workers goes back decades. And there are strong signs that the latest wave of criminal prosecutions might not mark the final chapter.
RELATED
Profiteering masquerades as medical care for injured California workers
The 102-year-old system is built on a simple bargain. Workers give up the right to sue for injuries sustained on the job. In exchange, about 15 million people covered by workers’ compensation insurance in California expect access to free and readily available medical care.
State officials focused on delivering care to workers neglected to build safeguards into the system, according to Dale Banda, a former head of enforcement for the California Department of Insurance.
“You’re dealing with a program that was designed from the beginning not to incorporate fraud as a component,” he said.
It took nearly 80 years for lawmakers to establish the California Department of Insurance’s Fraud Assessment Commission, which collects money from workers’ compensation insurers and distributes it to prosecutors who press the cases.
That was 1991. By then, the system had developed a culture of corruption.
The fraud was so blatant in 1993 that James Little, then president of a workers’ compensation insurance firm, worked with a colleague to pitch the story to television outlets.
“Primetime Live” wound up capturing footage of “cappers,” people paid to recruit patients. They trolled unemployment lines trying to lure laid-off workers to clinics. Journalists put hidden cameras in a fake workers’ comp clinic and recorded jockeying for kickbacks in exchange for patient referrals.
In 1993, “Primetime Live” recorded “cappers,” people paid to recruit patients for workers’ compensation clinics. The practice is illegal.
Credit: Primetime Live
The sham clinic’s leader, using the pseudonym Paul Morgan, confessed on camera that he wanted to help clean up the system – having participated in a half-billion dollars’ worth of fraud.
He recalled that when he was in business, recruiters brought his clinic so many uninjured workers that “we would be surprised and really didn’t know what to do with a person who came through with a legitimate injury.”
Little recalls the era: “It was way out of control.”
And it seemed to get even worse. The system costs more than doubled from $9.5 billion in 1995 to $25 billion in 2002.
In 2004, a state audit found across-the-board shortcomings in state officials’ efforts to measure and investigate workers’ compensation fraud.
That was when the new governor, Arnold Schwarzenegger, aimed his star power squarely at the problem of soaring workers’ compensation costs. He swept through Costco warehouse stores from Burbank to Sacramento with TV cameras trailing him, warning that the problem could force companies out of state.
Schwarzenegger brokered a reform deal with lawmakers that brought down costs, but it is difficult to tell whether it had an impact on fraud as well. State government leaders responsible for workers’ compensation long have struggled to measure the medical fraud problem.
The state’s Department of Insurance commissioned a 2008 study, which concluded that the state’s employers were footing the bill for up to $1.3 billion a year in erroneous payments. The report dealt with errors instead of fraud, it said, because identifying fraud would mean proving criminal intentions.
The overall “error rate” was about twice the current rate in Medicare and Medicaid.
Malcolm Sparrow, a Harvard University management professor, created the method that California officials used to reach the conclusions. He said in an interview that government officials must be willing to measure fraud to control it – and then make key changes. The next step, he said, is to conduct a follow-up study to see whether the errors are falling off.
“It takes a high degree of political courage to do a measurement program rigorously,” Sparrow said. “You have to be prepared to deal with the huge embarrassment” of failure.
RATHER LISTEN TO THE STORY?
Subscribe to the Reveal podcast to get this and other stories.
California officials never followed up using the same measurement, leaving no way to determine whether they have succeeded at reducing errors. Instead, the Department of Industrial Relations commissioned a study, unveiled last year, that used different methods to examine medical spending in workers’ compensation.
That study still found problems. Even though workers were not getting hurt worse or more often on the job, medical costs had climbed $1.6 billion from 2007 to 2012.
Barbara Wynn, a researcher with the Rand Corp., led that second study. Her preliminary findings suggest one significant cost driver was the overuse of MRI studies, particularly in Southern California. The MRIs, she said, often were done too early in the course of medical treatment to be clearly medically necessary.
Wynn’s discovery raises the specter that some of those MRIs might have been part of a scam to drum up business.
Indictments unsealed in January show that two firms specializing in MRIs were part of kickback schemes meant to guarantee a steady stream of patients. Since 2007, those MRI firms have billed insurers more than $260 million for services and filed more than 50,000 demands for payment, according to a Reveal analysis of state data.
Charges in that kickback case – dubbed “Operation Backlash” – mostly cover the years since 2012, when lawmakers passed another reform package. The new law added layers of medical review over doctors’ requests for treatment. It also took aim at middlemen who collect money on behalf of medical providers.
Recent cases in an FBI-led sting suggest that despite the legal changes, fraud continues to flourish. A San Diego prosecutor who handled one part of that case said it is merely a “small constellation in a universe of workers’ comp fraud.”
“This happens all over California,” said Pedro Bernal, the San Diego County deputy district attorney. “This is how it’s done.”
For more information:
https://www.facebook.com/Injured-Workers-N...
Added to the calendar on Fri, Apr 8, 2016 5:48PM
Add Your Comments
Comments
(Hide Comments)
San Francisco Labor Council Resolution on Workers Memorial Day 2016 – April 28, 2016
http://sflaborcouncil.org/wp-content/uploads/2016/04/04-11-16Resolution-On-Workers-Memorial-Day-2016-Ltrhd.pdf
Whereas, April 28 is commemorated worldwide as Workers Memorial Day; and Whereas, health and safety on the job is a basic labor and human right; and
Whereas, injured workers deserve good medical care and compensation for their injuries on the job; and
Whereas, California has less than 200 Cal OSHA inspectors for 18.5 million workers; and
Whereas, the deregulation of Workers Compensation in California through SB 899 and SB 863 has led to the injured workers being denied healthcare benefits due to anonymous doctors and an obstacle course call independent review decisions by an outsourced company called Maximus; and
Whereas, the insurance industry has controls the Workers Compensation system; and
Whereas, there is more and more use of opiates and growing addiction due to injured workers not getting medical treatment; and
Whereas, there has been a major increase in workplace bullying on the job leading to health and safety problems and forcing workers on disability and workers compensation; and
Whereas, Federal OSHA only has 2,000 OSHA inspectors for 130 million workers and only 500 investigators of those workers who have been retaliated for making OSHA complaints; and
Whereas, Federal OSHA management have not enforced the protection of OSHA whistleblowers and have bullied AFGE OSHA Whistleblower Protection Program WPP AFGE Local 2371members in Region 9; and
Whereas, Federal OSHA management and the Department of Labor management have only allowed a small percentage of whistleblowers to be protected with a merit determination; and
Whereas, Federal OSHA inspectors including SFLC delegate and fired Federal OSHA investigator Darrell Whitman who is also a member and steward of AFGE Local 2371 have been bullied, harassed and fired from the agency for doing their jobs; and
Whereas, if workers both union and unorganized are not protected from making health and safety complaints and there is not proper enforcement of Federal OSHA protection laws this is a threat to all workers and the public; and
Whereas, the protection of worker health and safety in transportation, energy, healthcare, construction, education, agriculture, biotech and many other industries is critical for these workers and the public; and
Whereas, the Workers Memorial Day on April 28, 2016 commemorates the workers who have died on the job and those workers who have been injured; and
Therefore be it Resolved the San Francisco Labor Council calls for proper staffing of OSHA in the Cal- OSHA program and Federal Osha program, the rehiring of fired Federal OSHA lawyer Darrell Whitman and an end to the harassment and bullying of AFGE OSHA Whistleblower Protection Program worker, support for a independent investigator to investigate the retaliation against Federal OSHA staff who have been bullied, retaliated and fired for doing their job; and
Be it Further Resolved the San Francisco Labor Council calls for the elimination of the Independent Medical Review system with anonymous doctors not even licensed in California that is being used to prevent injured workers from getting treatment and for the elimination of the insurance industry control of our workers compensation system and for full rehabilitation training for injured workers and laws preventing workplace bullying; and
Be it Further Resolved the San Francisco Labor Council will support and publicize the April 28, 2016 Workers Memorial Day at ILWU Local 34 at 7:00 PM in San Francisco sponsored by the Injured Workers National Network; and
Be it Finally Resolved the San Francisco Labor Council calls for concurrence by all affiliated bodies including the California Federation of Labor.
Submitted by Brenda Barros, SEIU 1021, and James Charos, SMART 1741, and unanimously adopted by the San Francisco Labor Council on April 11, 2016.
Respectfully,
Tim Paulson Executive Director
OPEIU 3 AFL-CIO 11
http://www.sflaborcouncil.org
Federal Agency OSHA That Protects Whistleblowers Accused of Retaliating Against One of its Own
http://www.fairwarning.org/2016/04/ex-whistleblower-investigator-blows-the-whistle-on-osha/
By Stuart Silverstein on April 11, 2016
Darrell Whitman, former whistleblower investigator for the U.S. Occupational Safety and Health Administration
For nearly five years, Darrell Whitman was a federal investigator who probed whistleblowers’ complaints about being fired or otherwise punished for exposing alleged corporate misconduct.
He wanted to help whistleblowers, viewing them as a crucial line of defense against employers who violated health and safety standards or wasted taxpayer dollars.
But now Whitman, 70, is blowing the whistle himself. And he is accusing the agency where he used to work, the Occupational Safety and Health Administration, the branch of the Labor Department whose duties include protecting whistleblowers.
Whitman, in a whistleblower claim filed last week with the U.S. Office of Special Counsel, charges that the San Francisco regional office of OSHA’s Whistleblower Protection Program routinely dumped legitimate complaints. What’s more, Whitman’s complaint says his disclosures to senior OSHA and Labor Department officials -– all the way up to Labor Secretary Thomas Perez — “did not spark good faith corrective action. Rather, they led to investigations of Mr. Whitman that eventually formed the basis for his termination” last May. He claims that three other investigators who protested the office’s practices also were fired or pushed out.
The result, Whitman claims, is that safety hazards and wasteful spending persist while whistleblowers often are silenced by employers that get away with illegal retaliation.
Whitman’s complaint largely tracks the concerns he raised in letters to federal officials (examples here and here) and in interviews with FairWarning and previously with KNTV (NBC in the Bay Area). He zeroes in on his former boss, Joshua Paul, and other officials in OSHA’s San Francisco regional office, which oversees California, Arizona, Nevada and Hawaii.
Sometimes, Whitman said, Paul ordered investigators to water down their findings or reversed the findings without explanation. In other instances, Whitman said, cases would be closed out after quickie investigations that barely examined the retaliation claims. Other times, he said, Paul dragged his feet in completing investigations for three years or more, apparently to put pressure on whistleblowers to settle.
‘The companies would scream bloody murder’
Whitman told FairWarning that those problems in San Francisco reflect a broader breakdown across the 10 regional OSHA offices that administer the whistleblower program. He maintains that the program often is too cozy with business to take on rogue employers. “There’s open hostility within OSHA to this program,” Whitman said.
If the program did its job, “the companies would scream bloody murder,” added Whitman, an attorney with a PhD in politics who has taught college, served as a campaign consultant and worked as a lawyer in government and private practice.
Whitman’s complaint calls for his reinstatement, back pay and damages, while also seeking an investigation of Paul “and any other relevant DOL [Department of Labor] officials.”
OSHA disputed Whitman’s allegations. In a written response, Jordan Barab, a Labor Department deputy assistant secretary, said: “To suggest that OSHA is not committed to protecting workers or that it is arbitrarily dismissing cases is not only absurd, it’s a huge disservice to the investigators who work hard to protect the rights of whistleblowers across the country. The Whistleblower Protection Program is a small staff with an enormous task, and that staff is committed, at every level of the organization, to protecting the rights of workers and to upholding the law.”
As for Paul, in November he moved from his job as senior investigator overseeing whistleblower investigations in San Francisco to a new role as coordinator of the region’s alternative dispute resolution program, which works on whistleblower cases. OSHA said the job change was unrelated to Whitman’s allegations. OSHA turned down a request for an interview with Paul, saying it “would not be appropriate” for him to respond to Whitman’s allegations.
OSHA is responsible for enforcing whistleblower provisions under 22 federal laws that cover everything from nuclear power plants and public transit to the trucking, railroad and airline industries.
But as Congress has assigned OSHA one category of workers after another, some critics say its staff has been swamped by the added workload, creating incentives to dismiss cases to keep up.
Jordan Barab, deputy assistant secretary of Labor.
Whitman’s complaint cites six cases that he says were mishandled. One involved a nuclear plant official who said he lost his job after discussing security problems with the Nuclear Regulatory Commission.
Another case involved Michael Madry. He was a Phoenix-based quality assurance specialist for EMLab P&K, which describes itself as North America’s “leading commercial indoor air quality testing laboratory.”
According to court records, Madry, 51, was promoted to quality assurance manager at EMLab in May 2008. Over the next year, Madry received reports from outside auditors questioning the accuracy of the firm’s asbestos testing as well as complaints from lab analysts about being pressured to rush through asbestos tests.
Madry investigated, focusing on the company’s San Bruno, Calif., lab, which tested for asbestos at schools and for the U.S. Navy and other customers. He became increasingly concerned about the accuracy of tests, and repeatedly raised the issue with company officials.
Soon he began getting poor performance reviews and, according to court records, the company president complained in an internal memo of his “emotional outbursts and obvious instability.”
On Sept. 30, 2010, soon after being put on medical leave by a psychiatrist, Madry filed his whistleblower complaint.
Whitman investigated and in July 2011 found that the complaint had merit. But then the case languished.
As Whitman recounts in his own complaint, Paul delayed action for almost a year by requiring four rewrites of his merit findings, and also pushed for Madry to accept “a nuisance settlement.” According to Whitman, after he complained to OSHA chief David Michaels, Paul removed Whitman from the case. Whitman told FairWarning that he eventually saved the case by going over his boss’ head and getting the whistleblower program’s national director to step in.
‘The system, it doesn’t work’
Three years of legal skirmishes followed for Madry. As a Nov. 16 trial before an administrative law judge was about to begin, Madry reached a settlement totaling $122,500 with EMLab. The company declined to comment after the settlement but, in an earlier interview, an EMLab spokesperson gave a blanket denial of Madry’s claims, without discussing specifics.
The struggle, in Madry’s view, wasn’t worth it. “I wouldn’t recommend anybody do what I did, just because the system, it doesn’t work,” he said.
“Here I am, more than five years later,” he added, “and I’m no better off than when I filed my complaint.”
Michael Madry, a whistleblower who raised questions about the accuracy of his company’s asbestos testing.
Nilgun Tolek, who headed OSHA’s whistleblower program until 2011, said she wasn’t familiar with the evidence behind Whitman’s allegations. However, she cautioned against assuming that when an administrator overturns an investigator’s finding there is “ill intent.”
“It’s always the case that what the investigator recommends in a report is subject to further review and may not end up holding water in the end. It’s not an individual person’s report. It’s the agency’s report, and it has to go through all kinds of review,” Tolek said.
Although Whitman’s case is novel for OSHA, it’s not the only time whistleblower defenders have been accused of mistreating their own employees. Two lawyers formerly with the National Whistleblowers Center, a nonprofit legal group in Washington, in late 2014 received an undisclosed sum to settle their complaints (here and here) that the organization fired them and also retaliated against other employees who tried to unionize. The settlement came shortly before a National Labor Relations Board administrative law judge was set to hear the case. The National Whistleblowers Center did not admit any wrongdoing.
Flawed investigations by OSHA’s Whistleblower Protection Program and growing case backlogs were cited last fall in a report by the Labor Department’s inspector general.
In an audit tracking October 2012 through March 2014, the inspector general found problems in 24 of 132 randomly selected complaints. Among other deficiencies, investigators failed to contact complainants’ witnesses and to give complainants the time needed to provide evidence.
OSHA also failed to meet deadlines on 3,206 of the 4,475 complaints it received that warranted investigations. The investigations took an average of 238 days to complete, up from 150 days in 2010, when previous federal audits lambasted the agency for poor performance.
OSHA management, in response, acknowledged that improvements were needed. But the agency also noted that the number of new complaints climbed to 3,060 in the 2014 fiscal year, up 58 percent from 2005.
“Consequently, OSHA still lacks the resources that it needs to process and investigate whistleblower complaints with the expedience that we would like, while also maintaining the quality and thoroughness that is appropriate,” the agency said.
- See more at: http://www.fairwarning.org/2016/04/ex-whistleblower-investigator-blows-the-whistle-on-osha/#sthash.ioS3uPF3.dpuf
WW 3-29-16 OSHA Chief Michaels and DOL Secretary Perez In Corruption Scandal With OSHA Whistleblower Darrell Whitman And Fired OSHA Manager Adam Finkel
https://soundcloud.com/workweek-radio/ww3-29-16-osha-dol-manager-corruption-with-darrell-whitman-and-adam-finkel
WorkWeek looks at the growing corruption scandal at the Department of Labor DOL and OHSA. We interview fired OSHA investigator and lawyer Darrell Whitman who is a steward in AFGE Local 2371 and Adam Finkel who is a OSHA management whistleblower and was fired from OSHA. He now is a Senior Fellow and Executive Director of Penn Program on Regulation, University of Pennsylvania.
They discuss the nearly complete failure of OSHA and the Whistleblower Protection Program to defend health and safety whistleblowers and also the criminal collusion between OSHA, DOL and the AJL with corporations they are supposed to regulate. Whitman discusses the role of ALJ Judge Steven B. Berlin who criminally colluding with Test America/H.I.G. Capital to limit their liability in the retaliation against OSHA whistleblower Michael Madry who was a Quality Assurance Manager at Test America which is owned by H.I.G. Capital. He was bullied, terrorized and fired by Test America/H.I.G. Capital after exposing massive fraudulent testing of toxic dump sites like San Francisco Hunters Point Naval Shipyard and Treasure Island. According to Whitman tens of thousands of test results on asbestos and other toxins were fraudulent and this was kept a secret by OSHA and the DOL putting the public in danger. He also reports that OSHA chief David Michaels and DOL secretary Tom Perez were personally involved in a criminal conspiracy to cover up his firings and those of other AFGE workers in the Region 9 office of OSHA Whistleblower Protection Program.
Adam Finkel talks about the role of the management in seeking to shutdown the protection of OSHA whistleblowers and the lack of accountability.
Further media and info:
http://www.dailycensored.com/ohsagate/
https://youtu.be/lfr7rtfqeFc
https://youtu.be/08OY7kMydSs
https://www.youtube.com/watch?v=WA0nLj6sZ5Y
https://www.youtube.com/edit?o=U&video_id=3gotQhC1lHE
https://www.youtube.com/watch?v=FQiB7bGHFas
https://www.youtube.com/watch?v=x3PTf6F887Q
https://soundcloud.com/workweek-radio/ww6-2-15-osha-lawyer-darrell-whitman-interviewed-part-1
https://soundcloud.com/workweek-radio/ww6-9-15-osha-lawyer-darrell-whitman-interviewed-part-2
https://www.youtube.com/watch?v=FQiB7bGHFas
https://www.youtube.com/watch?v=kQ3zii0T3z4
http://www.oalj.dol.gov/Decisions/ALJ/TSC/2013/MADRY_MICHAEL_J_v_EMLAB_PandK_LLC_2013TSC00001_(OCT_09_2015)_130744_ORDER_PB.PDF#search=michael%20madry
http://www.cc.com/episodes/xiptmz/the-daily-show-with-jon-stewart-february-26--2015---olivia-wilde-season-20-ep-20067
http://www.nbcbayarea.com/investigations/OSHA-Whistleblower-Investigator-Blows-Whistle-on-Own-Agency–293711041.html
Production of WorkWeek Radio
workweek [at] kpfa.org
https://soundcloud.com/workweek-radio
Whistleblower Protection Program & Fired WPP OSHA Investigator Lawyer Darrell Whitman With GAP Louis Clark
https://www.youtube.com/watch?v=WA0nLj6sZ5Y
Louis Clark, lawyer and co-founder of the Government Accountability Project GAP in Washington DC discusses the Whistleblower Protection Project and how it is working including the affect of deregulation and privatization of government agencies that protect health and safety and the environment..
The Whistleblower Protection Program WPP is supposed to protect Federal whistleblowers throughout the United States government. He also talks about the systemic corruption in the Department of Labor DOL and OSHA and the retaliation and firing of OSHA WPP investigator, lawyer and AFGE Local 2371 steward Darrell Whitman. Clark talks about the problem of bullying of AFGE members in San Francisco OSHA Region 9 office who were seeking to protect workers who were retaliated for doing their jobs and faced retaliation themselves by the management. He also discusses reports that OSHA officials met privately with Lockheed Martin, Test America H.I.G. Capital, PG&E and other companies to criminally collude to dismiss merit complaints and coerce bad settlements for workers retaliated against for whistleblowing. He discusses the potential criminal obstruction of justice by top government officials including ALJ judges who are aware of the corruption charges and conspired to cover them up.
He also discusses the efforts of GAP to develop rules that will be enforced to protect all government whistleblowers including in the financial industry to prevent another financial crisis like 2008.
This interview was done on March 10, 2016 in San Franciso by KPFA WorkWeek journalist Steve Zeltzer
For more information:
Government Accountability Project
http://www.whistleblower.org
http://www.dailycensored.com/ohsagate/
https://soundcloud.com/workweek-radio/ww6-2-15-osha-lawyer-darrell-whitman-interviewed-part-1
https://soundcloud.com/workweek-radio/ww6-9-15-osha-lawyer-darrell-whitman-interviewed-part-2
https://soundcloud.com/workweek-radio/ww3-17-15-osha-corruption-with-madry-and-usw-oil-strike
https://www.youtube.com/watch?v=lfr7rtfqeFc
https://www.youtube.com/watch?v=3gotQhC1lHE
https://www.youtube.com/watch?v=08OY7kMydSs
https://www.youtube.com/watch?v=kQ3zii0T3z4
https://www.youtube.com/watch?v=kQ3zii0T3z4
https://www.indybay.org/newsitems/2015/10/28/18779351.php
HIG TestAmerica
http://higcapital.com/portfolio/company/98
http://www.mintpressnews.com/federal-whistleblower-investigator-fired-after-blowing-the-whistle-on-his-own-agency/210347/
Madry Court Cases
http://www.oalj.dol.gov/Decisions/ALJ/TSC/2013/MADRY_MICHAEL_J_v_EMLAB_PandK_LLC_2013TSC00001_(OCT_09_2015)_130744_ORDER_PB.PDF#search=michael%20madry
http://www.cc.com/episodes/xiptmz/the-daily-show-with-jon-stewart-february-26--2015---olivia-wilde-season-20-ep-20067
http://www.nbcbayarea.com/investigations/OSHA-Whistleblower-Investigator-Blows-Whistle-on-Own-Agency–293711041.html
Production of Labor Video Project
http://www.laborvideo.org
http://sflaborcouncil.org/wp-content/uploads/2016/04/04-11-16Resolution-On-Workers-Memorial-Day-2016-Ltrhd.pdf
Whereas, April 28 is commemorated worldwide as Workers Memorial Day; and Whereas, health and safety on the job is a basic labor and human right; and
Whereas, injured workers deserve good medical care and compensation for their injuries on the job; and
Whereas, California has less than 200 Cal OSHA inspectors for 18.5 million workers; and
Whereas, the deregulation of Workers Compensation in California through SB 899 and SB 863 has led to the injured workers being denied healthcare benefits due to anonymous doctors and an obstacle course call independent review decisions by an outsourced company called Maximus; and
Whereas, the insurance industry has controls the Workers Compensation system; and
Whereas, there is more and more use of opiates and growing addiction due to injured workers not getting medical treatment; and
Whereas, there has been a major increase in workplace bullying on the job leading to health and safety problems and forcing workers on disability and workers compensation; and
Whereas, Federal OSHA only has 2,000 OSHA inspectors for 130 million workers and only 500 investigators of those workers who have been retaliated for making OSHA complaints; and
Whereas, Federal OSHA management have not enforced the protection of OSHA whistleblowers and have bullied AFGE OSHA Whistleblower Protection Program WPP AFGE Local 2371members in Region 9; and
Whereas, Federal OSHA management and the Department of Labor management have only allowed a small percentage of whistleblowers to be protected with a merit determination; and
Whereas, Federal OSHA inspectors including SFLC delegate and fired Federal OSHA investigator Darrell Whitman who is also a member and steward of AFGE Local 2371 have been bullied, harassed and fired from the agency for doing their jobs; and
Whereas, if workers both union and unorganized are not protected from making health and safety complaints and there is not proper enforcement of Federal OSHA protection laws this is a threat to all workers and the public; and
Whereas, the protection of worker health and safety in transportation, energy, healthcare, construction, education, agriculture, biotech and many other industries is critical for these workers and the public; and
Whereas, the Workers Memorial Day on April 28, 2016 commemorates the workers who have died on the job and those workers who have been injured; and
Therefore be it Resolved the San Francisco Labor Council calls for proper staffing of OSHA in the Cal- OSHA program and Federal Osha program, the rehiring of fired Federal OSHA lawyer Darrell Whitman and an end to the harassment and bullying of AFGE OSHA Whistleblower Protection Program worker, support for a independent investigator to investigate the retaliation against Federal OSHA staff who have been bullied, retaliated and fired for doing their job; and
Be it Further Resolved the San Francisco Labor Council calls for the elimination of the Independent Medical Review system with anonymous doctors not even licensed in California that is being used to prevent injured workers from getting treatment and for the elimination of the insurance industry control of our workers compensation system and for full rehabilitation training for injured workers and laws preventing workplace bullying; and
Be it Further Resolved the San Francisco Labor Council will support and publicize the April 28, 2016 Workers Memorial Day at ILWU Local 34 at 7:00 PM in San Francisco sponsored by the Injured Workers National Network; and
Be it Finally Resolved the San Francisco Labor Council calls for concurrence by all affiliated bodies including the California Federation of Labor.
Submitted by Brenda Barros, SEIU 1021, and James Charos, SMART 1741, and unanimously adopted by the San Francisco Labor Council on April 11, 2016.
Respectfully,
Tim Paulson Executive Director
OPEIU 3 AFL-CIO 11
http://www.sflaborcouncil.org
Federal Agency OSHA That Protects Whistleblowers Accused of Retaliating Against One of its Own
http://www.fairwarning.org/2016/04/ex-whistleblower-investigator-blows-the-whistle-on-osha/
By Stuart Silverstein on April 11, 2016
Darrell Whitman, former whistleblower investigator for the U.S. Occupational Safety and Health Administration
For nearly five years, Darrell Whitman was a federal investigator who probed whistleblowers’ complaints about being fired or otherwise punished for exposing alleged corporate misconduct.
He wanted to help whistleblowers, viewing them as a crucial line of defense against employers who violated health and safety standards or wasted taxpayer dollars.
But now Whitman, 70, is blowing the whistle himself. And he is accusing the agency where he used to work, the Occupational Safety and Health Administration, the branch of the Labor Department whose duties include protecting whistleblowers.
Whitman, in a whistleblower claim filed last week with the U.S. Office of Special Counsel, charges that the San Francisco regional office of OSHA’s Whistleblower Protection Program routinely dumped legitimate complaints. What’s more, Whitman’s complaint says his disclosures to senior OSHA and Labor Department officials -– all the way up to Labor Secretary Thomas Perez — “did not spark good faith corrective action. Rather, they led to investigations of Mr. Whitman that eventually formed the basis for his termination” last May. He claims that three other investigators who protested the office’s practices also were fired or pushed out.
The result, Whitman claims, is that safety hazards and wasteful spending persist while whistleblowers often are silenced by employers that get away with illegal retaliation.
Whitman’s complaint largely tracks the concerns he raised in letters to federal officials (examples here and here) and in interviews with FairWarning and previously with KNTV (NBC in the Bay Area). He zeroes in on his former boss, Joshua Paul, and other officials in OSHA’s San Francisco regional office, which oversees California, Arizona, Nevada and Hawaii.
Sometimes, Whitman said, Paul ordered investigators to water down their findings or reversed the findings without explanation. In other instances, Whitman said, cases would be closed out after quickie investigations that barely examined the retaliation claims. Other times, he said, Paul dragged his feet in completing investigations for three years or more, apparently to put pressure on whistleblowers to settle.
‘The companies would scream bloody murder’
Whitman told FairWarning that those problems in San Francisco reflect a broader breakdown across the 10 regional OSHA offices that administer the whistleblower program. He maintains that the program often is too cozy with business to take on rogue employers. “There’s open hostility within OSHA to this program,” Whitman said.
If the program did its job, “the companies would scream bloody murder,” added Whitman, an attorney with a PhD in politics who has taught college, served as a campaign consultant and worked as a lawyer in government and private practice.
Whitman’s complaint calls for his reinstatement, back pay and damages, while also seeking an investigation of Paul “and any other relevant DOL [Department of Labor] officials.”
OSHA disputed Whitman’s allegations. In a written response, Jordan Barab, a Labor Department deputy assistant secretary, said: “To suggest that OSHA is not committed to protecting workers or that it is arbitrarily dismissing cases is not only absurd, it’s a huge disservice to the investigators who work hard to protect the rights of whistleblowers across the country. The Whistleblower Protection Program is a small staff with an enormous task, and that staff is committed, at every level of the organization, to protecting the rights of workers and to upholding the law.”
As for Paul, in November he moved from his job as senior investigator overseeing whistleblower investigations in San Francisco to a new role as coordinator of the region’s alternative dispute resolution program, which works on whistleblower cases. OSHA said the job change was unrelated to Whitman’s allegations. OSHA turned down a request for an interview with Paul, saying it “would not be appropriate” for him to respond to Whitman’s allegations.
OSHA is responsible for enforcing whistleblower provisions under 22 federal laws that cover everything from nuclear power plants and public transit to the trucking, railroad and airline industries.
But as Congress has assigned OSHA one category of workers after another, some critics say its staff has been swamped by the added workload, creating incentives to dismiss cases to keep up.
Jordan Barab, deputy assistant secretary of Labor.
Whitman’s complaint cites six cases that he says were mishandled. One involved a nuclear plant official who said he lost his job after discussing security problems with the Nuclear Regulatory Commission.
Another case involved Michael Madry. He was a Phoenix-based quality assurance specialist for EMLab P&K, which describes itself as North America’s “leading commercial indoor air quality testing laboratory.”
According to court records, Madry, 51, was promoted to quality assurance manager at EMLab in May 2008. Over the next year, Madry received reports from outside auditors questioning the accuracy of the firm’s asbestos testing as well as complaints from lab analysts about being pressured to rush through asbestos tests.
Madry investigated, focusing on the company’s San Bruno, Calif., lab, which tested for asbestos at schools and for the U.S. Navy and other customers. He became increasingly concerned about the accuracy of tests, and repeatedly raised the issue with company officials.
Soon he began getting poor performance reviews and, according to court records, the company president complained in an internal memo of his “emotional outbursts and obvious instability.”
On Sept. 30, 2010, soon after being put on medical leave by a psychiatrist, Madry filed his whistleblower complaint.
Whitman investigated and in July 2011 found that the complaint had merit. But then the case languished.
As Whitman recounts in his own complaint, Paul delayed action for almost a year by requiring four rewrites of his merit findings, and also pushed for Madry to accept “a nuisance settlement.” According to Whitman, after he complained to OSHA chief David Michaels, Paul removed Whitman from the case. Whitman told FairWarning that he eventually saved the case by going over his boss’ head and getting the whistleblower program’s national director to step in.
‘The system, it doesn’t work’
Three years of legal skirmishes followed for Madry. As a Nov. 16 trial before an administrative law judge was about to begin, Madry reached a settlement totaling $122,500 with EMLab. The company declined to comment after the settlement but, in an earlier interview, an EMLab spokesperson gave a blanket denial of Madry’s claims, without discussing specifics.
The struggle, in Madry’s view, wasn’t worth it. “I wouldn’t recommend anybody do what I did, just because the system, it doesn’t work,” he said.
“Here I am, more than five years later,” he added, “and I’m no better off than when I filed my complaint.”
Michael Madry, a whistleblower who raised questions about the accuracy of his company’s asbestos testing.
Nilgun Tolek, who headed OSHA’s whistleblower program until 2011, said she wasn’t familiar with the evidence behind Whitman’s allegations. However, she cautioned against assuming that when an administrator overturns an investigator’s finding there is “ill intent.”
“It’s always the case that what the investigator recommends in a report is subject to further review and may not end up holding water in the end. It’s not an individual person’s report. It’s the agency’s report, and it has to go through all kinds of review,” Tolek said.
Although Whitman’s case is novel for OSHA, it’s not the only time whistleblower defenders have been accused of mistreating their own employees. Two lawyers formerly with the National Whistleblowers Center, a nonprofit legal group in Washington, in late 2014 received an undisclosed sum to settle their complaints (here and here) that the organization fired them and also retaliated against other employees who tried to unionize. The settlement came shortly before a National Labor Relations Board administrative law judge was set to hear the case. The National Whistleblowers Center did not admit any wrongdoing.
Flawed investigations by OSHA’s Whistleblower Protection Program and growing case backlogs were cited last fall in a report by the Labor Department’s inspector general.
In an audit tracking October 2012 through March 2014, the inspector general found problems in 24 of 132 randomly selected complaints. Among other deficiencies, investigators failed to contact complainants’ witnesses and to give complainants the time needed to provide evidence.
OSHA also failed to meet deadlines on 3,206 of the 4,475 complaints it received that warranted investigations. The investigations took an average of 238 days to complete, up from 150 days in 2010, when previous federal audits lambasted the agency for poor performance.
OSHA management, in response, acknowledged that improvements were needed. But the agency also noted that the number of new complaints climbed to 3,060 in the 2014 fiscal year, up 58 percent from 2005.
“Consequently, OSHA still lacks the resources that it needs to process and investigate whistleblower complaints with the expedience that we would like, while also maintaining the quality and thoroughness that is appropriate,” the agency said.
- See more at: http://www.fairwarning.org/2016/04/ex-whistleblower-investigator-blows-the-whistle-on-osha/#sthash.ioS3uPF3.dpuf
WW 3-29-16 OSHA Chief Michaels and DOL Secretary Perez In Corruption Scandal With OSHA Whistleblower Darrell Whitman And Fired OSHA Manager Adam Finkel
https://soundcloud.com/workweek-radio/ww3-29-16-osha-dol-manager-corruption-with-darrell-whitman-and-adam-finkel
WorkWeek looks at the growing corruption scandal at the Department of Labor DOL and OHSA. We interview fired OSHA investigator and lawyer Darrell Whitman who is a steward in AFGE Local 2371 and Adam Finkel who is a OSHA management whistleblower and was fired from OSHA. He now is a Senior Fellow and Executive Director of Penn Program on Regulation, University of Pennsylvania.
They discuss the nearly complete failure of OSHA and the Whistleblower Protection Program to defend health and safety whistleblowers and also the criminal collusion between OSHA, DOL and the AJL with corporations they are supposed to regulate. Whitman discusses the role of ALJ Judge Steven B. Berlin who criminally colluding with Test America/H.I.G. Capital to limit their liability in the retaliation against OSHA whistleblower Michael Madry who was a Quality Assurance Manager at Test America which is owned by H.I.G. Capital. He was bullied, terrorized and fired by Test America/H.I.G. Capital after exposing massive fraudulent testing of toxic dump sites like San Francisco Hunters Point Naval Shipyard and Treasure Island. According to Whitman tens of thousands of test results on asbestos and other toxins were fraudulent and this was kept a secret by OSHA and the DOL putting the public in danger. He also reports that OSHA chief David Michaels and DOL secretary Tom Perez were personally involved in a criminal conspiracy to cover up his firings and those of other AFGE workers in the Region 9 office of OSHA Whistleblower Protection Program.
Adam Finkel talks about the role of the management in seeking to shutdown the protection of OSHA whistleblowers and the lack of accountability.
Further media and info:
http://www.dailycensored.com/ohsagate/
https://youtu.be/lfr7rtfqeFc
https://youtu.be/08OY7kMydSs
https://www.youtube.com/watch?v=WA0nLj6sZ5Y
https://www.youtube.com/edit?o=U&video_id=3gotQhC1lHE
https://www.youtube.com/watch?v=FQiB7bGHFas
https://www.youtube.com/watch?v=x3PTf6F887Q
https://soundcloud.com/workweek-radio/ww6-2-15-osha-lawyer-darrell-whitman-interviewed-part-1
https://soundcloud.com/workweek-radio/ww6-9-15-osha-lawyer-darrell-whitman-interviewed-part-2
https://www.youtube.com/watch?v=FQiB7bGHFas
https://www.youtube.com/watch?v=kQ3zii0T3z4
http://www.oalj.dol.gov/Decisions/ALJ/TSC/2013/MADRY_MICHAEL_J_v_EMLAB_PandK_LLC_2013TSC00001_(OCT_09_2015)_130744_ORDER_PB.PDF#search=michael%20madry
http://www.cc.com/episodes/xiptmz/the-daily-show-with-jon-stewart-february-26--2015---olivia-wilde-season-20-ep-20067
http://www.nbcbayarea.com/investigations/OSHA-Whistleblower-Investigator-Blows-Whistle-on-Own-Agency–293711041.html
Production of WorkWeek Radio
workweek [at] kpfa.org
https://soundcloud.com/workweek-radio
Whistleblower Protection Program & Fired WPP OSHA Investigator Lawyer Darrell Whitman With GAP Louis Clark
https://www.youtube.com/watch?v=WA0nLj6sZ5Y
Louis Clark, lawyer and co-founder of the Government Accountability Project GAP in Washington DC discusses the Whistleblower Protection Project and how it is working including the affect of deregulation and privatization of government agencies that protect health and safety and the environment..
The Whistleblower Protection Program WPP is supposed to protect Federal whistleblowers throughout the United States government. He also talks about the systemic corruption in the Department of Labor DOL and OSHA and the retaliation and firing of OSHA WPP investigator, lawyer and AFGE Local 2371 steward Darrell Whitman. Clark talks about the problem of bullying of AFGE members in San Francisco OSHA Region 9 office who were seeking to protect workers who were retaliated for doing their jobs and faced retaliation themselves by the management. He also discusses reports that OSHA officials met privately with Lockheed Martin, Test America H.I.G. Capital, PG&E and other companies to criminally collude to dismiss merit complaints and coerce bad settlements for workers retaliated against for whistleblowing. He discusses the potential criminal obstruction of justice by top government officials including ALJ judges who are aware of the corruption charges and conspired to cover them up.
He also discusses the efforts of GAP to develop rules that will be enforced to protect all government whistleblowers including in the financial industry to prevent another financial crisis like 2008.
This interview was done on March 10, 2016 in San Franciso by KPFA WorkWeek journalist Steve Zeltzer
For more information:
Government Accountability Project
http://www.whistleblower.org
http://www.dailycensored.com/ohsagate/
https://soundcloud.com/workweek-radio/ww6-2-15-osha-lawyer-darrell-whitman-interviewed-part-1
https://soundcloud.com/workweek-radio/ww6-9-15-osha-lawyer-darrell-whitman-interviewed-part-2
https://soundcloud.com/workweek-radio/ww3-17-15-osha-corruption-with-madry-and-usw-oil-strike
https://www.youtube.com/watch?v=lfr7rtfqeFc
https://www.youtube.com/watch?v=3gotQhC1lHE
https://www.youtube.com/watch?v=08OY7kMydSs
https://www.youtube.com/watch?v=kQ3zii0T3z4
https://www.youtube.com/watch?v=kQ3zii0T3z4
https://www.indybay.org/newsitems/2015/10/28/18779351.php
HIG TestAmerica
http://higcapital.com/portfolio/company/98
http://www.mintpressnews.com/federal-whistleblower-investigator-fired-after-blowing-the-whistle-on-his-own-agency/210347/
Madry Court Cases
http://www.oalj.dol.gov/Decisions/ALJ/TSC/2013/MADRY_MICHAEL_J_v_EMLAB_PandK_LLC_2013TSC00001_(OCT_09_2015)_130744_ORDER_PB.PDF#search=michael%20madry
http://www.cc.com/episodes/xiptmz/the-daily-show-with-jon-stewart-february-26--2015---olivia-wilde-season-20-ep-20067
http://www.nbcbayarea.com/investigations/OSHA-Whistleblower-Investigator-Blows-Whistle-on-Own-Agency–293711041.html
Production of Labor Video Project
http://www.laborvideo.org
For more information:
http://sflaborcouncil.org/wp-content/uploa...
We are 100% volunteer and depend on your participation to sustain our efforts!
Get Involved
If you'd like to help with maintaining or developing the website, contact us.
Publish
Publish your stories and upcoming events on Indybay.
Topics
More
Search Indybay's Archives
Advanced Search
►
▼
IMC Network